INTRODUCTION:
Worldwide there is an increasing adoption of Descemet membrane endothelial keratoplasty (DMEK) representing a major shift in the treatment
paradigm for Fuchs’ endothelial dystrophy and other forms of endothelial dysfunction. Studies on DMEK have demonstrated better visual outcomes, faster visual rehabilitation, and a significantly lower incidence of rejection compared with its predecessors, Descemet stripping endothelial keratoplasty (DSEK) and Penetrating keratoplasty. Despite these advantages most of the corneal surgeons in India have been slow to adopt DMEK, in part because DSEK still remains an excellent procedure, but also owing to what has been described as the steep learning curve of DMEK.
METHODS:
Three key challenges for the DMEK surgeon are 1.Stripping the donor DM, 2. Transferring & Handling the fragile Descemet’s membrane and 3. Placement and proper orientation of the graft in the anterior chamber. During stripping the donor DM, a small tear can cause wastage of the tissue. The problem does not end there. Once the DM is stripped it characteristically scrolls with the endothelial side out configuration, thus making it unsafe to handle the tissue. Further, the dark pigmented brown eyes in Indian patients gives less contrast while in the anterior chamber when compared with non-pigmented western eyes. Adding to the difficulty is that the tissue orientation is not easily visualized through hazy diseased corneas. For all of these reasons, discerning the correct orientation of a DMEK graft in the anterior chamber can be a challenge and accidental placement of upside-down grafts remains a cause of iatrogenic primary graft failure in DMEK even in the hands of experienced DSEK surgeons. A number of groups worldwide have developed orientation techniques, including the use of various external light sources, intra-cameral instrumentation of the graft scroll, and modifications to the graft itself.
RESULTS:
We initially started doing DMEK in 2013. 47 patients completed 1 year follow-up. Even though the best corrected visual acuity drastically improved in all the cases, what was worrying us was the percentage of endothelial cell loss (ECL) and the failure and complication rate. The mean ECL at 6 months and 1 year were 24% and 31% respectively. The complication rate was 28 % and the successful outcome was 83% in this group. This unpredictable outcome after DMEK, is the main reason why not even a few corneal surgeons in India are venturing into this technique.
OUR TECHNIQUE TO SIMPLIFY DMEK
We thought it necessary to improvise this technique and address these limitations. We developed and validated three novel methods. 1. Single Pull technique for donor DM removal 2. Prototype DM Injector 3. Stromal-sided L-stamp. These three unique innovations by us provides definitive and intuitive technique to strip, transfer and orient the DM intra operatively before elevating the DM with air bubble inside the anterior chamber.
Further after improvising the technique we performed DMEK in 40 eyes of 39 patients. These patients were followed up to 6 months and the results are as follows:
SUMMARY OF RESULTS WITH OUR IMPROVISED TECHNIQUE FOR DMEK
| DATA SUMMARY | ||||||
| Age | 65+/-11.5 | Male | 65+/-12.1 | |||
| Female | 66+/- 9.1 | p>0.05 | ||||
| Gender | ||||||
| Male | 82% | |||||
| Female | 18% | |||||
| Indication | ||||||
| PBK | 68% | |||||
| BK | 10% | |||||
| ABK | 3% | |||||
| Fuch’s | 20% | |||||
| Mean LOG MARG Visual Acuity | ||||||
| PRE OP | 1.257+/0.441 | p<0.001 | ||||
| POST OP | 0.265+/0.398 | |||||
| Lines Improved | ||||||
| Nil | 8% | |||||
| 1 – 3 | 13% | |||||
| 4 – 6 | 60% | |||||
| > 6 | 20% | |||||
| Mean ECD | ||||||
| PRE OP | 2191+/-292 | p<0.001 | ||||
| POST OP | 1854+/-294 | |||||
| ECD Difference | 328+/-36 | |||||
|
Loss % |
15.1% | |||||
| Complication | ||||||
| YES | 5% | |||||
| NO | 95% | |||||
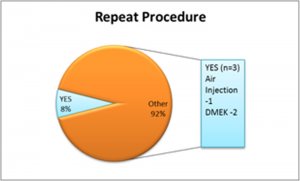
| Repeat Procedure | ||||||
| YES | 8% | |||||
| NO | 92% | |||||
| OUT COME | ||||||
| SUCCESS | 92% | |||||
| FAILURE | 8% | |||||
DISCUSSION:
Endothelial cell loss at 6-month follow-up period was 27.9±16.0% after DMEK in a study reported by Terry MA et al study. Theofilas and associates reported an endothelial cell loss of 41% in the DMEK group at 6-month post-operative period. Price et al reported eEndothelial cell loss was of 32% ± 20% after DMEK in 38 eyes that reached the 6-month examination in Price et al study. Recently in 2015, Gorovoy et all reported an endothelial cell loss of 19% at 1 year follow up.
Our modified technique , has shown the least endothelial cell loss and failure rates compared to the above studies, thus simplifying the procedure and stressing the importance of a making a standardized protocol to achieve a favourable outcome so that many corneal surgeons in India can confidently start DMEK .
CONCLUSION:
DMEK will definitely be the procedure of choice for endothelial diseases in future and it is high time we adopt standard and simple techniques to increase the success of DMEK.

