Dr.Bhramaramba Banagar, B16981. Dr. PukhrajRishi
Introduction
The meibomian glands in the eyelids, which synthesize and secrete lipids for the superficial tear film layer, play an important role in maintaining a healthy ocular surface through reducing tear evaporation . Dysfunction of meibomian glands, characterized by obstruction of gland orifices, changes of glandular secretion (meibum) and lid margins, leads to alternation of lipid layer and tear film instability, which may cause a variety of ocular surface disorders, in particularly, dry eye.
Meibography provides photographic documentation of the meibomian gland under specialized illumination techniques. Normal meibomian glands appear as grapelike clusters with acini. In the non-contact technique, a camera and light source do not touch the patient during the meibography procedure. Non-contact meibography was first introduced by Arita et al. in 2008. Their non-contact meibograph consists of a slitlamp microscope equipped with an Infrared (IR)charge-coupled device video camera and an IR transmitting filter to allow the observation of the everted lid (but without contact with a light probe with the everted lids being directly illuminated by IR light). The light and dark contrast of the meibomian glands is opposite that of the transilluminationtechnique in that they appear light instead of dark. The potential advantage of this technique is that it is more comfortable for patients, in addition to the fact that this system is now commercially available in some markets as additional equipment for the Topcon slitlamp microscope. A normal IR-CCD (mention fullform)video camera including an IR light source was reported in 2011 to be a useful alternative for non-contact meibography. This set-up consisted of an IR CCD video-camera (pixel: PAL: 628(H) × 582(V), ¼″ CCD Sensor, 802CHA CCD( authors to mention fullforms); Shenzhen LYD Technology Co. Ltd, Shenzhan, China) and near focus adaptation by a +20 diopter lens and was named the Portable Non-Contact Meibography.
In this study we used smart phone (which smart phone) for meibographic imaging along with infrared light which consisted of infrared bulb that illuminates the meibomian glands. The infrared mode (negative mode) along with magnification and high resolution of smart phone is used to capture meibomian gland images. The eye lid is everted , infrared light is illuminated on the glands and image is taken with smart phone in infrared mode. The above image can be saved in smart phone , transmitted to other devices wirelessly , The images were analysed using Image J software. The number of meibomian gland drop –out was calculated.
Aim of study
- To evaluate the morphologic assessment and quantification of the meibomain glands using non contact method by smart phone.
- To evaluate the relationship between meibmain gland morphology with tear function tests.
Methodology
Subjects recruited in this study
・ 100 subjects attending clinic for general health check up were included in the study.
(The data used in this study were obtained from the right eye in each subject.)
・ Males: 62 , females: 38
・ Mean age 46.5 ±15.4 years (range 19~75 years)
Exclusion criteria
Current contact lens wearer
Has any ocular disease
Is using any topical medications that may affect ocular health
Has known sensitivity to the diagnostic pharmaceuticals to be used in the study
Clearance was taken from the Ethics Committee of the institute. Subjects were informed about the test and consent was taken .
Study method-
OSDI questionnairewas provided to patients and their response was analysed and OSDI Score given.
The following tear function tests were conducted. All examinations were completed on a separated day, and evaluated in the same darkened room by the same ophthalmologist.
Tear function tests
Schirmer test Ⅰ
Break-up time of tear film (BUT)
Fluorescein staining score (FS)
The tear film BUT was calculated for a mean value after 3 successive measurements, the value of Schirmer I test was calculated on the moist length of the strip. Corneal fluorescein staining was graded from 0 to 12, a sum of the scores of corneal four quadrants, which were scored individually as 0 (no staining), 1 (mild staining with a few scattered dots of stains), 2 (moderate staining between 1 and 3), and 3 (severe staining with confluent stains or corneal filaments)
Evaluation of meibomian gland dysfunction.
The morphological characteristics and function of meibomian glands and gland dropout degree visualized by meibography using smart phone The digital images obtained by meibography were recorded and analyzed using image J software. . This following meibomian gland dropout degree was graded for each eyelid as meiboscore : grade 0 (no loss of meibomian glands), grade 1 (loss ,33% of the whole glands area), grade 2 (loss area between 33% and 67%), and grade 3 (loss .67% of the whole area). The meiboscore of each eye was calculated as the sum of the scores from both upper and lower eyelids, which made the total meiboscore per eye to a range of 0–6.
RESULTS
Fig 1.-Meibography image taken with the everted lower eyelid .Meibomain glands seen as darkened structures ,acni resembling grape like structures
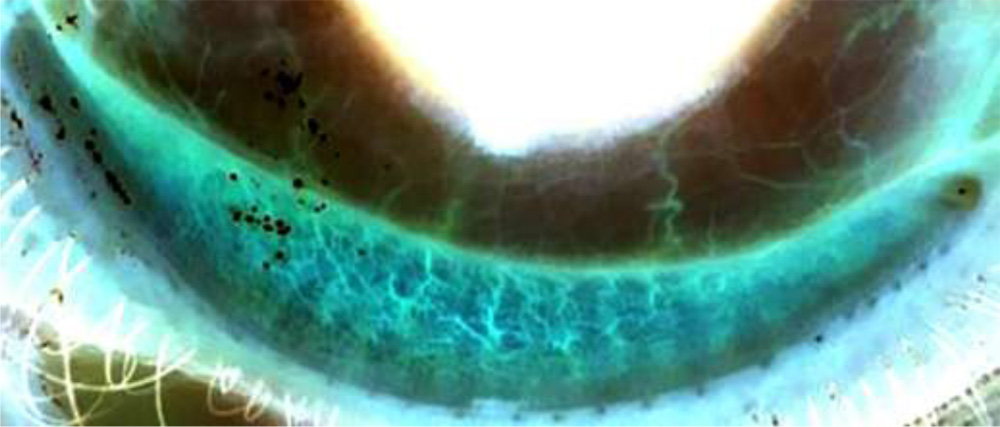
Fig 2.- Image showing gray area indicating gland dropout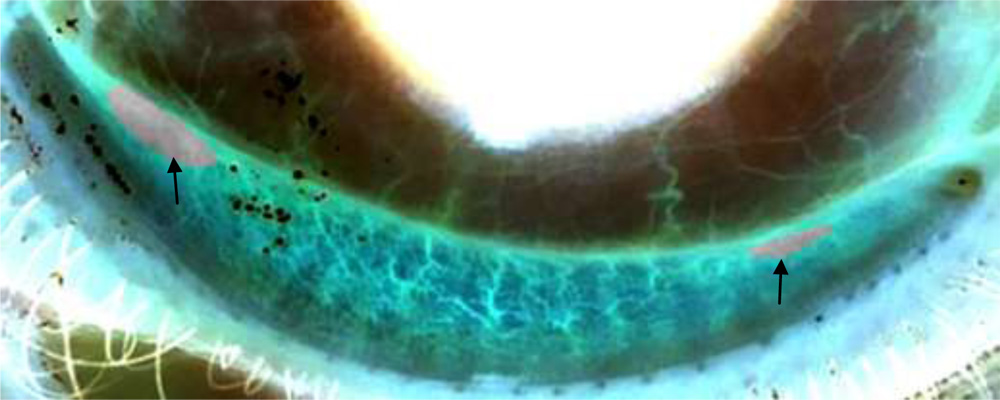
Fig 3.- Image analysed using Image J software. Gray area indicates gland dropout.
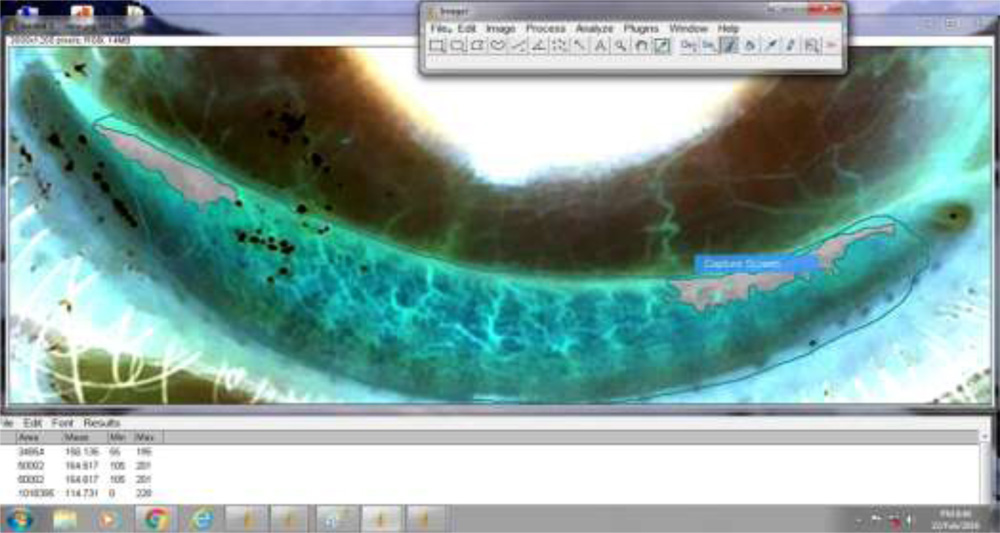
Statistical analysis.
The Pearson and Spearman tests were performed to determine correlations between meibomain gland morphologic values and tear function test parameters.
Results-
Table 1.-Correlations of meiboscore with dry eye parameters
| R ( correlation ) | P value | Mean | |
| OSDI | 0.052 | 0.484 | 37.92+18.27 |
| Fluorescein score | 0.402 | 0.005 | 3.67+2.87 |
| BUT (s) | 0.382 | 0.005 | 4.73+1.78 |
| Schirmer I (mm) | 0.021 | 0.776 | 11.53±8.32 mm |
| Age | 0.412 | 0.001 | 46.5 ±15.4 years |
| Sex | 0.032 | 0.654 |
Meibomian gland dysfunction parameters were strongly positively correlated and fluorescein score (P<0.0001),inversely correlated with TBUT (P<0.05. However meibomian gland dysfunction parameters and fluorescein score didnot correlate with Schirmer test values.
DISCUSSION
The result of our study in respect to morphological changes in meibomian glandswith age and sex correlatedwith the results of studies by Nichols et al , Foulks et al, Dogru M, et al.
Our study results in respect to Schirmers test , TBUT , Fluorescein score correlated with results of Miller KL, Walt JG, Mink DR.
Conclusion
Non-contact infrared meibography using smart phone offers a useful tool for obtaining a morphological analysis of the meibomian glands in ocular surface evaluation.
REFERENCES
- Arita R, et al. Noncontact infrared meibography to document age-related changes of the meibomian glands in a normal population. Ophthalmology. 2008 ;115:911-5.
- Arita R, et al. Contact lens wear is associated with decrease of meibomian glands. Ophthalmology. 2009 ;116:379-84.
- Arita R, et al. Proposed diagnostic criteria for obstructive meibomian gland dysfunction. Ophthalmology. 2009 ;116:2058-63.
- Den S, et al. Association between meibomian gland changes and aging, sex, or tear function. Cornea. 2006 ;25:651-5.
- Obata H. Anatomy and histopathology of human meibomian gland. Cornea. 2002 ;21::S70-4

