Dr. Suchit Dadia, D19186, Dr.Akshay Nair, Dr. Shruti Shirwadkar, Dr. (Mrs ) PotdarNayana Anil
TITLE: Use of maternal upperarm skin allograft in surgical management of bilteral cicatrical ectropion in a case of congenital lamellar ichthyosis
Dadia SD1 ,Nair AG2 ,Potdar NA2 ,Shinde CA3
ABSTRACT
Ichthyosis includes a spectrum of rare dystrophic inherited skin disorders with presentation ranging from birth till late childhood with characteristic excessive scaling of skin.
We present a case of a 2 year old male child, brought by parents that came with complaints of scaling of skin around eyes, outward turning of all four lids and inability to close eyes completely since birth. He was a diagnosed case of congenital lamellar ichthyosis. The patient was on treatment with oral retinoids and topical keratolytics application over the skin. Early exposure keratopathy was noted with anterior lamellar shortening of all four lids, causing contracture and ectropion. Anterior lamellar reconstruction was performed for both eyelids of each eye using a maternal upper arm allograft. At 2 months follow-up the graft was well apposed, ectropion was corrected and patient could completely close his eyes preventing further risk of corneal damage.
key words: lamellar ichthyosis, ectropion, exposure keratopathy, allograft
INTRODUCTION
Ichthyosis is an inherited group of skin disorders characterized by skin thickening and scale formation.
The congenital ichthyotic disorders are divided into four main types. These are (i) ichthyosis vulgaris (ii) X-linked ichthyosis (iii) bullous ichthyosiform erythroderma (BIE) or epidermolytic hyperkeratosis and (iv) non bullous ichthyosiform erythroderma (NBIE) and lamellar ichthyosis (LI).
The main ocular associations of congenital ichthyosis are corneal opacities and ectropion of the lids.Ectropion occurs only in the lamellar type of ichthyosis and Arnold first reported this association in 1834. It is frequently bilateral and the lower lid is more severely affected.Mechanism for ectropion formation is cited to be severe drying of skin with subsequent inflammation,scarring and contracture of lids. Affected patients are born as collodion babies, i.e. encased in a taut, shiny membrane at birth that evolves into typical scale like lesions over a few days to weeks.
Unlike other varieties of ichthyosis,in the lamellar variant skin flexures,palms and soles are also affected, suggesting involvement of the entire body,precluding the use of autografts.
We present a case of congenital lamellar ichthyosis with bilateral cicatrical ectropion that had to be managed surgically.
CASE REPORT
A 2 year old male child, brought by his parents reported with complaints of outward-turning of all four lids and inability to close both eyes completely since birth. The baby was delivered at 37 weeks of gestation through normal vaginal delivery and was kept in NICU for 7 days due to physiological jaundice. He was covered in a collodion membrane at birth which was followed a few weeks later by a generalized scaling rash. The baby was the 3rd child and his parents were second degree relatives. However, there was no family history of skin problems and his two elder siblings were both normal.
His parents complained of gradual upturning of eyelids since 10 days of age with increased scaling of the skin with time. He was under the care of a dermatologist since 1 month of age and was on oral retinoids, hydroxyzine, topical fusidin cream and physiogel lotion for the skin and topical lubricants and keratolytics for the eye. He was referred to our oculoplasty clinic at 2 years of age with bilateral upper and lower lid cicatrical ectropion(figure 1).
His visual acuity was 6/9 in both eyes (Lea symbols) with pupils briskly reacting to light. Lid closure was incomplete and there was punctuate corneal staining indicating exposure. Bell’s phenomenon was good to excellent. Posterior segment findings were within normal limits.
In view of incomplete lid closure,exposure keratopathy,increasing outward turning of eyelids despite possible medical/nonsurgical management,a decision to surgically correct the ectropion was made.
There were no areas of skin unaffected by the scaling process. Considering the age of the patient, no available autologous healthy skin, easy availability of maternal skin and economic constraints, ectropion repair using maternal allograft was planned in our patient.
Full thickness maternal skin allograft from the upper arm area was taken(figure 2), divided into 4 parts and anterior lamellar reconstruction of all the 4 lids was carried out in the same sitting. Skin closure was achieved using 6-0 prolene sutures(figure 3).. No postoperative immunosuppressive agents were given.
The postoperative course at 8 weeks follow up has been uneventful. Complete lid closure is now possible and there is no sign of corneal exposure(figure 4). No signs of graft rejection/failure were noted.
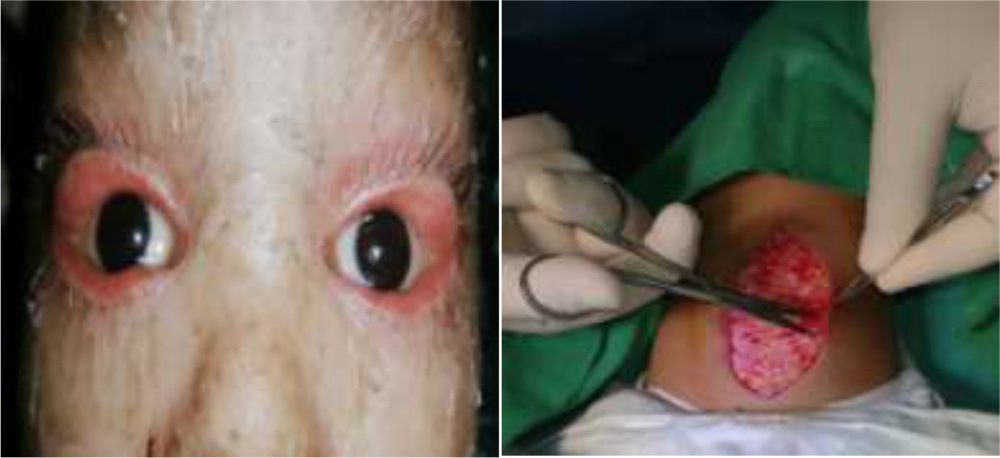
 (Clockwise from top left) figure1:bilateral cicatrical ectropion. figure2:maternal autograft harvest
(Clockwise from top left) figure1:bilateral cicatrical ectropion. figure2:maternal autograft harvest
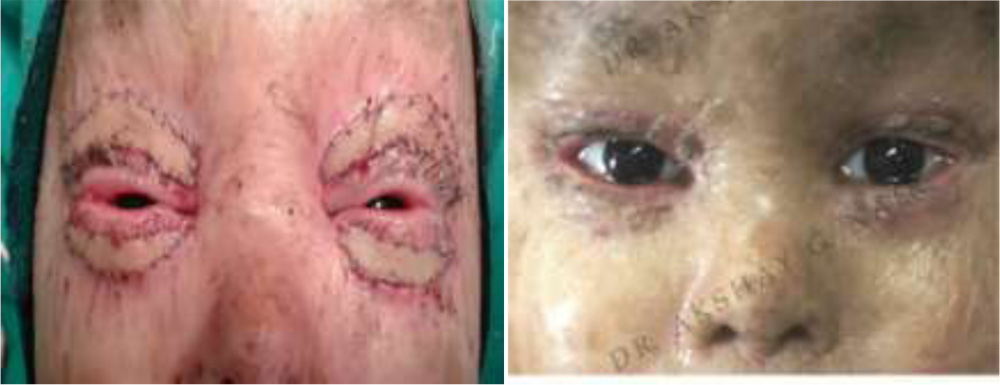
figure3:postop day 1 with all 4 grafts in situ. figure4:well apposed grafts at 2 months follow up.
DISCUSSION:
Lamellar ichthyosis is a rare, autosomal recessive, genetic disorder with great phenotypic variability. It is the least common, more severe form of congenital ichthyoses (incidence 1 in 5,00,000 births) with cicatrical ectropion as the most common presenting symptom. Management of patients with ichthyosis requires a team approach consisting of neonatologists, dermatologists and ophthalmologists and prompt referral to specialized ophthalmology centers is crucial to avoid the risk of serious ocular complications of ichthyosis like severe exposure keratopathy, limbal stem cell deficiency and spontaneous corneal perforation.
Although surgical repair of ectropion is the mainstay of treatment with outcomes of surgical procedures being good to excellent, there have been reports of cases managed conservatively by topical lubrication and tazarotene that showed significant spontaneous improvement of the ectropion. Both autogenous and allogenous grafts have been tried previously, such as penile foreskin, groin, post auricular, mucous membrane graft and engineered human skin (APLIGRAF) with variable results.
Use of maternal skin allograft is a safe and excellent approach to treat cicatrical ectropion in cases of congenital lamellar ichthyosis. To the best of our knowledge, this is the second documented case report where such an approach has been used.
REFERENCES:
1)Maternal skin allograft for cicatricial ectropion in congenital icthyosis.
Das S1, Honavar SG, Dhepe N, Naik MN. Ophthal Plast Reconstr Surg. 2010 Jan-Feb;26(1):42-3.
2) UTHOFF D, GORNEY M, TEICHMANN C. CICATRICIAL ECTROPION IN ICHTHYOSIS: A NOVEL APPROACH TO TREATMENT. OPH- THAL PLAST RECONSTR SURG 1994; 10: 92-5.
3)Chakraborti, C., Tripathi, P., Bandopadhyay, G., and Mazumder, D.B. Congenital bilateral ectropion in lamellar ichthyosis. Oman J Ophthalmol. 2011; 4: 35–36
4)CULICAN, S. AND MUSTER, P.L. REPAIR OF CICATRICIAL ECTROPION IN AN INFANT WITH HARLEQUIN ICHTHYOSIS USING ENGINEERED HUMAN SKIN. AM J OPHTHALMIC. 2002; 134: 442–443
5) Doss RP, Conn H, Tenzel DP. Cicatricial ectropion in lamellar ichthyosis. Ophthal Plast Reconstr Surg 1990; 6: 38-41.
6) Griffiths WAD, Judge MR, Leigh IM. Disorders of keratinisation. In: Champion RH, Burton JL, Burns DA, Breath- nach SM, editors. Rook/Wilkinson/Ebling Textbook of Dermatology. 6th ed. Vol 2. Oxford: Blackwell Science, 1998; 1483-588.
7) Lentz CL, Altman J. Lamellar ichthyosis. The natural clinical course of collodion baby. Arch Dermatol 1968; 97: 3-13.
8) Shindle RD, Leone CR Jr. Cicatricial ectropion associated with lamellar ichthyosis. Arch Ophthalmol 1973; 89: 62-4.
9) Zagora E. Operative treatment of severe cicatricial ectropion. Br J Ophthalmol 1967; 51: 94-6.
10) Peled I, BarLev A, Wexler MR. Surgical correction of ectropion in lamellar ichthyosis. Ann Plast Surg 1982; 8: 429-31.
11) Sigurdsson, H. and Baldursson, B.T. Inverting sutures with systemic retinoid and lubrication can correct ectropion in ichthyosis. Ophthal Plast Reconstruct Surg. 2014;

