Dr.Siddhartha Singh, S18715, Dr. Supriya Dabir, Dr.Manoj Khatri, Dr. Mohan Rajan
Presenting Author: Dr. Siddhartha Singh
Co- Authors: Dr. SupriyaDabir
Dr. Manoj Khatri
Dr. Mohan Rajan
INTRODUCTION
Cataract surgery is the most commonly performed ocular surgery in the world. Post-operativeEndophthalmitis is a rare but a very serious and devastating complication of cataract surgery. A Rapid survey done by NPCB during 2006-2007 showed a decrease in prevalence of blindness from 1.1 %( 2001-02) to 1 %( 2006-07) still cataract held the highest percentage (62.6%) as the main cause of blindness1. Visual outcomes after Endophthalmitis are poor, one third of the individuals do not gain vision better than counting fingers, and 50% do not recover vision better than 20/402.
Currently the confirmation of diagnosis of bacterial Endophthalmitis is dependent on the microbiological isolation of organisms and as time to microbiological diagnosis can vary between 2 and 12 days, the initial treatment of this disease necessarily requires the use of broad spectrum antibiotics to cover the full range of potential microbial pathogens.
The use of intraocular antibiotics in conjunction with systemic antimicrobials known to penetrate the blood ocular barrier has gained wide acceptance for the treatment of suspected bacterial Endophthalmitis.
The aim of the study was To Study Clinical & Microbiological profile of Post-operative Endophthalmitis affecting visual outcome.
MATERIALS AND METHODS
All cases of suspected post-surgical Endophthalmitis presenting to Rajan Eye Hospital were eligible for this study.Intraocular (aqueous and/or vitreous) sampling was undertaken on every patient along with ultrasound B scan. All samples were sent for grams stain, KOH, PCR, culture. Once the vitreous sample had been taken, vancomycin (1.0 mg in 0.1 ml) and amikacin (0.4 mg in 0.1 ml) were injected separately into the vitreous cavity through the same injection site. If Vitritis worsened Pars plana vitrectomy with intraocular antibiotics was performed. Cultures were maintained for 14 days. If no organism was isolated the case was considered culture negative even if organisms were thought to be present on the smear. The data collected included age, gender, type of surgery, any complication during the surgery, time interval to the onset of endophthalmitis, visual acuity at presentation, diagnostic procedures performed, culture results, management.
RESULTS
Twentypost-surgical cases were enrolled into the study which included 18 post phacoemulsification, 1 phacoemulsification with Trabeculectomy and 1 post penetrating keratoplasty.
- Mean age of presentation was 62 years (range 46- 72 years) with Male: Female ratio of 11: 9.
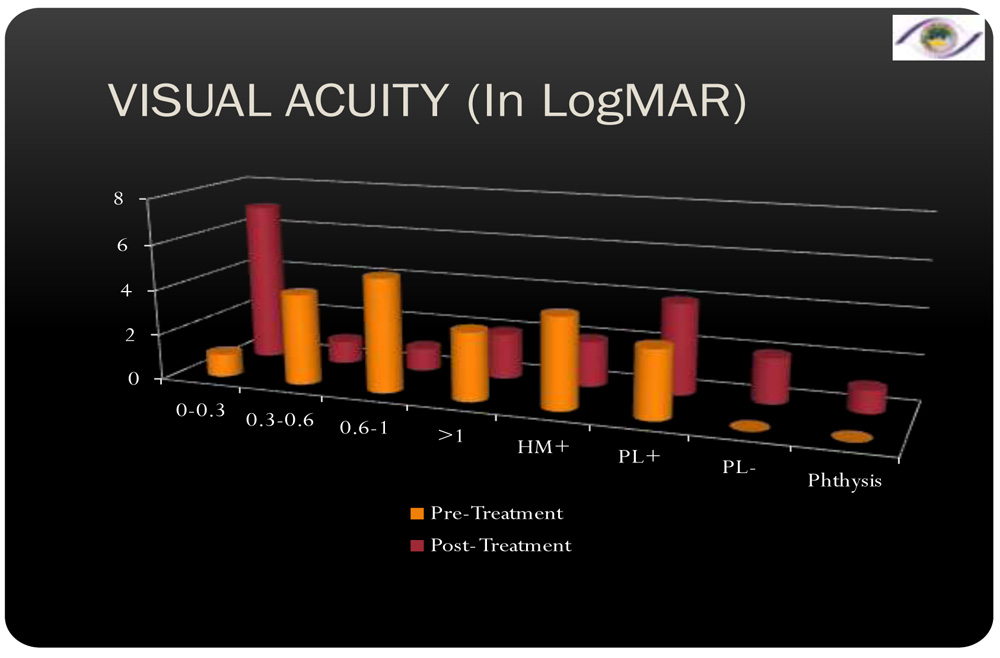
- Presenting Best Corrected Visual Acuity ranged from 0.3 logMAR to Perception of light.
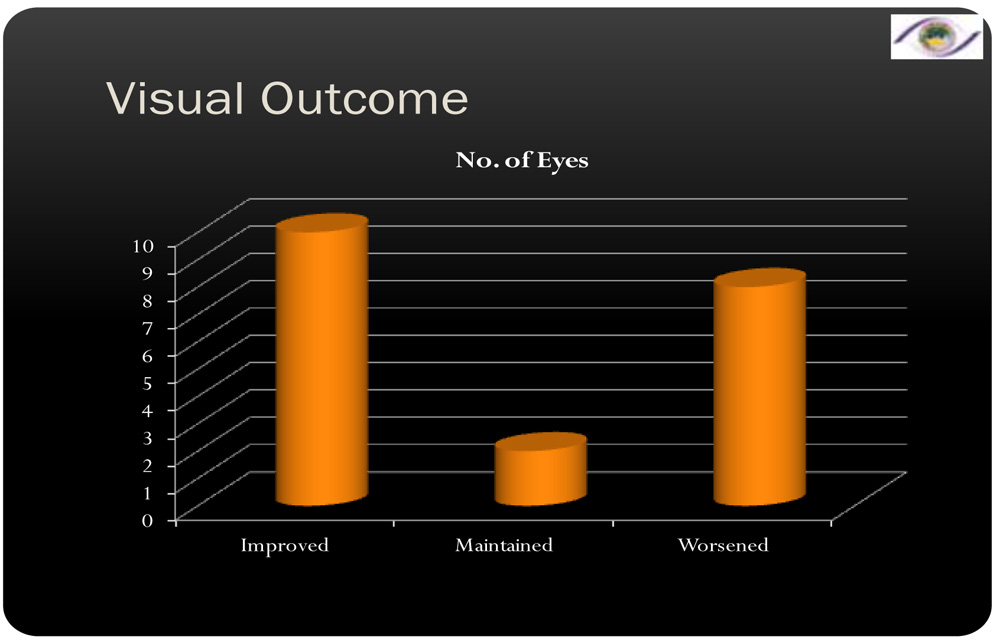
- Improvement in Best Corrected Visual Acuity of more than 2 lines was seen in 50% of the patients. 40% of the patients worsened. 10% of the patients maintained the same visual acuity.
- Time of presentation ranged from 1 day to 7 years. Of this 6 patients presented within 10 days from the day of surgery
- Polymerase Chain Reaction was positive for Eubacteria in all the cases, 4 cases had Panfungal positive& 9 cases were positive for Propionibacterium acnes.
-
DISCUSSION:
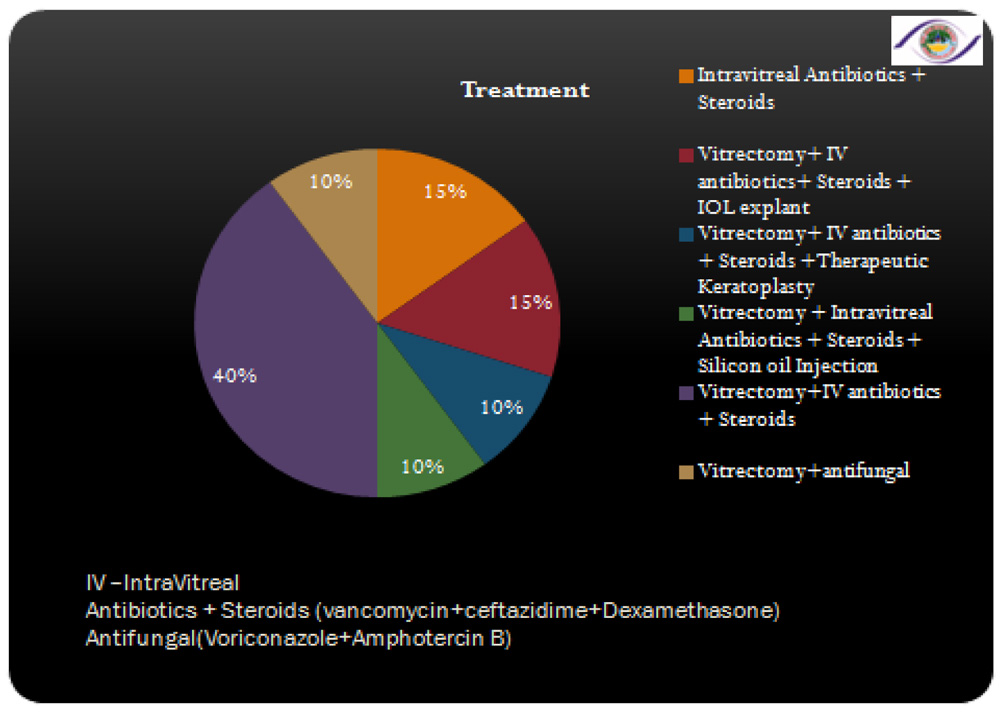
Since most of the bacterial causing post-operative endophthalmitis reside in the patients’ fornix, eyelid and conjunctiva3, 4; pre-operative disinfection of peri-ocular surface is effective for prophylaxis. In one study it concluded that preoperative povidone–iodine is the single most effective means for reducing the risk for postoperative endophthalmitis5.Full coverage of all possible pathogens is mandatory in the treatment of presumed bacterial endophthalmitis and has been achieved by using a combination of vancomycin, amikacin, and ciprofloxacin. Intravitreal Voriconazole and Amphotericin-B in cases of suspected and positive cases of fungal endophthalmitis was given. Despite this coverage, however, the prognosis for a good visual outcome remains poor. The emerging resistance to vancomycin is of concern and should be carefully monitored.
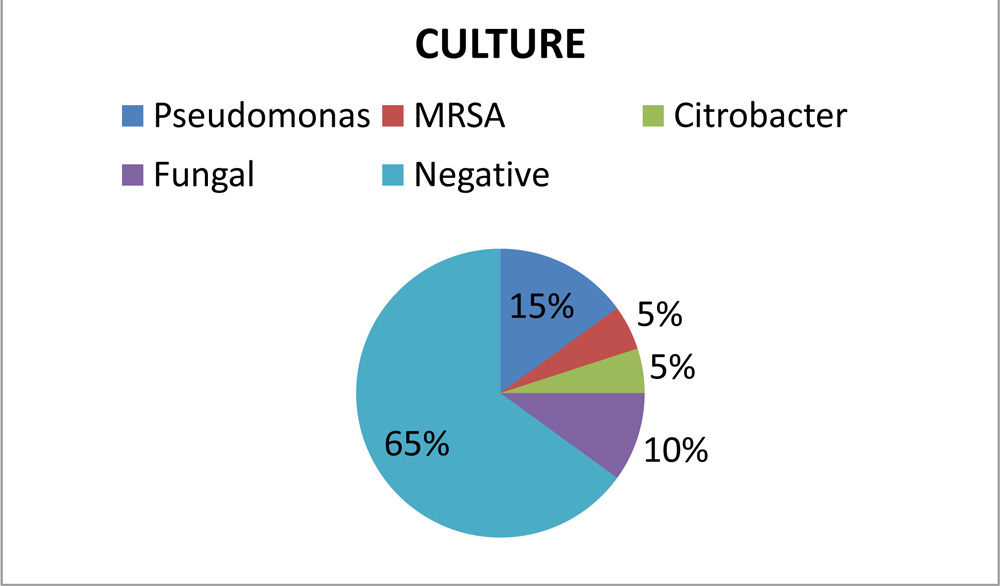
In this study only 35% of the cases were culture positive which is less when compared to other studies (Endophthalmitis Vitrectomy Study that had 67% culture-positive cases6, study conducted by Aravind eye hospital which had 53% of culture positive cases7.)
Visual outcomes depend on microbial factors.Fungal endophthalmitis had a poor outcome and citrobacter related endophthalmitis was the most difficult to treat and lead to phthisisbulbi.Early diagnosis and aggressive management yielded favorable outcomes.
REFERENCES:
- National Programme for Control of Blindness, Ministry of Health & Family Welfare, Government of India [Internet]. Npcb.nic.in. 2016. Available from: http://npcb.nic.in/#.
- Lalwani G, Flynn H, Scott I, Quinn C, Berrocal A, Davis J et al. Acute-Onset Endophthalmitis after Clear Corneal Cataract Surgery (1996–2005). Ophthalmology. 2008;115(3):473-476.
- Keay, L., Gower, E.W., Cassard, S.D. et al.Postcataract surgery endophthalmitis in the United States: analysis of the complete 2003 to 2004 Medicare database of cataract surgeries. Ophthalmology. 2012; 119: 914–922.
- Results of the Endophthalmitis Vitrectomy Study. A randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Endophthalmitis Vitrectomy Study Group.Arch Ophthalmol. 1995; 113: 1479–1496.
- Ciulla, T.A., Starr, M.B., and Masket, S.Bacterial endophthalmitis prophylaxis for cataract surgery: an evidence-based update. Ophthalmology. 2002; 109: 13–24.
- Endophthalmitis Vitrectomy Study Group.Results of the Endophthalmitis Vitrectomy Study (a randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis). Arch Ophthalmol. 1995; 113: 1479–1496.
- Lalitha, P., Rajagopalan, J., Prakash, K. et al,Postcataractendophthalmitis in south India (Incidence and outcome). Ophthalmology. 2005;112:1884–1890.

