Dr. Prakash Chipade,
C14867, Dr. Vijay Shetty, Dr. Suhas Haldipurkar,
Dr. Devendra Phalak
Chief and Presenting author- Dr Prakash Chipade
Co-authors – Dr Suhas Haldipurkar
Dr Vijay Shetty
Dr Devendra Phalak
Financial Disclosure
Authors have no financial interest in this presentation
Introduction
- Calculation of intraocular lens power in High myope (HM) remains a challenge often leading to unexpected post operative refractive error. (1) (2)
- The main potential sources of errors in IOL calculation for HM eyes includes
- AL measurement – erroneous AL measurement in
presence of posterior staphyloma.
- IOL power calculation formula because it misjudge effective lens position(ELP)
- Adi Abulafia et al. J Cataract Refract Surgery 2015, 41:548-56
- P Szurman et al J Cataract Refract Surgery 2009, 35:1575-81
Aim of study
To compare accuracy of Barrett, SRK-T, and Holladay formulae in IOL power calculation in high myopic patients
Methods
- Method – Secondary data analysis
- Site –Tertiary eye care (Laxmi eye institute,panvel)
- Duration- April 2011 to March 2016
- Sample size – 40 eyes of 31 high myopic patients who undergone uneventful cataract surgery with PCIOL in the bag implantation were taken
Inclusion criteria
- Patients undergone uneventful cataract surgery with axial length >27mm measured by optical biometer(IOL master)
- Post operative BCVA >6/12
- 8mm clear corneal incision located temporally
Exclusion criteria
- Previous intraocular surgery other than cataract.
- Pre existing ocular diseases that may influence the post operative refraction, including keratoconus, corneal scarring, endothelial dystrophy, Retinal detachment
Methods
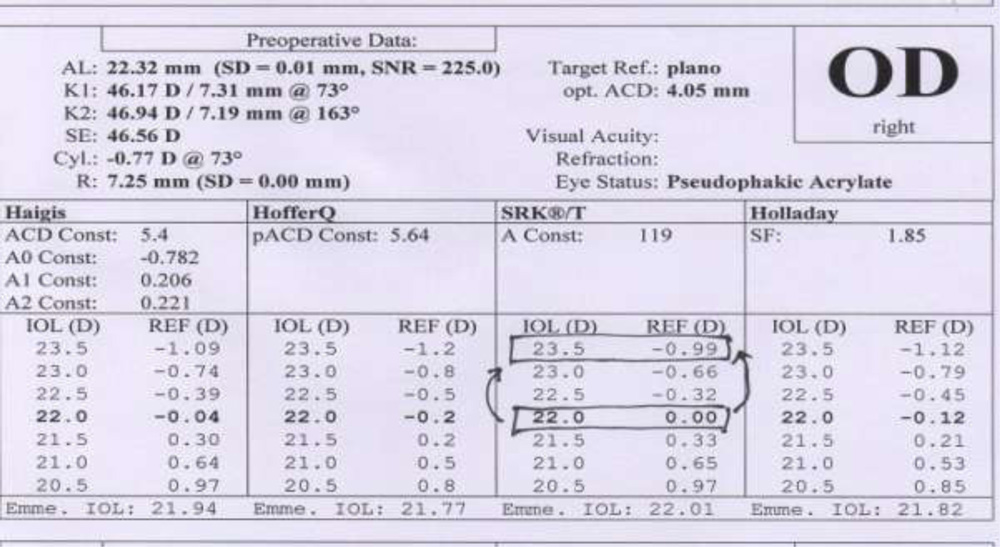
- The patients AL, anterior chamber depth (ACD) and keratometric (K1& K2) values were retrived from records for calculation of formulas.
- The post operative refraction at 4 weeks was noted .
- Spherical equivalent was calculated using above refraction.
- SRK-T, Holladay formulas were calculated using IOL master.
- The calculation with Barrett universal 2 formulas were performed using online software ((http://apacrs.org/barrett universal2/);
- The predicted IOL power for each formula was taken as target refraction of 0 or first myopic reading closest to 0.
- Ideal IOL power was calculated by using formula 1.5 x Spherical equivalent of post op refractive error and this figure was added to IOL implanted.
- Eg: IOL power implanted 15D,
Post op refraction = -2.00D
Ideal IOL power = -2 x 1.5 = -3.00
15 + (-3.00)= 12 D
The refractive prediction error was calculated the difference between the ideal IOL power and predicted IOL power.
- High myope patients were divided into 3 subsets
- Axial length between 27.18mm to 29.05mm
- Axial length between 29.14mm to 31mm
- Axial length between 31.56 to 33mm.
- Standard error of prediction is calculated across all three groups by all three formulas and compared using Kruskal-Wallis test and statistical analysis was done by using Stata version 13.
Results
40 eyes of 31 patients with mean age 50.9 (SD:9.08) were analysed
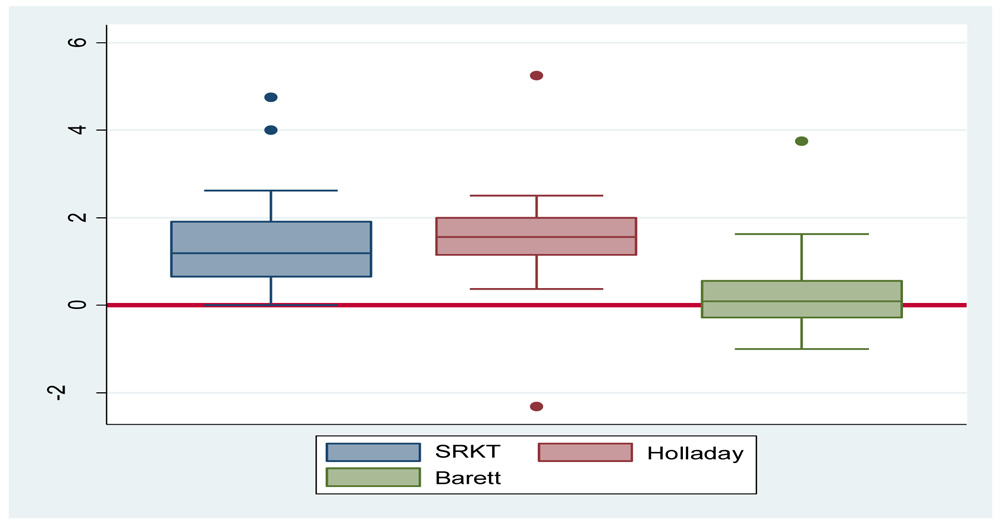
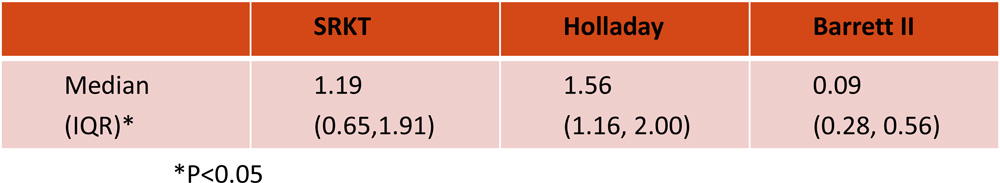
Box plot showing median error of IOL power with SRK-T, Holladay and Barrett II formula.
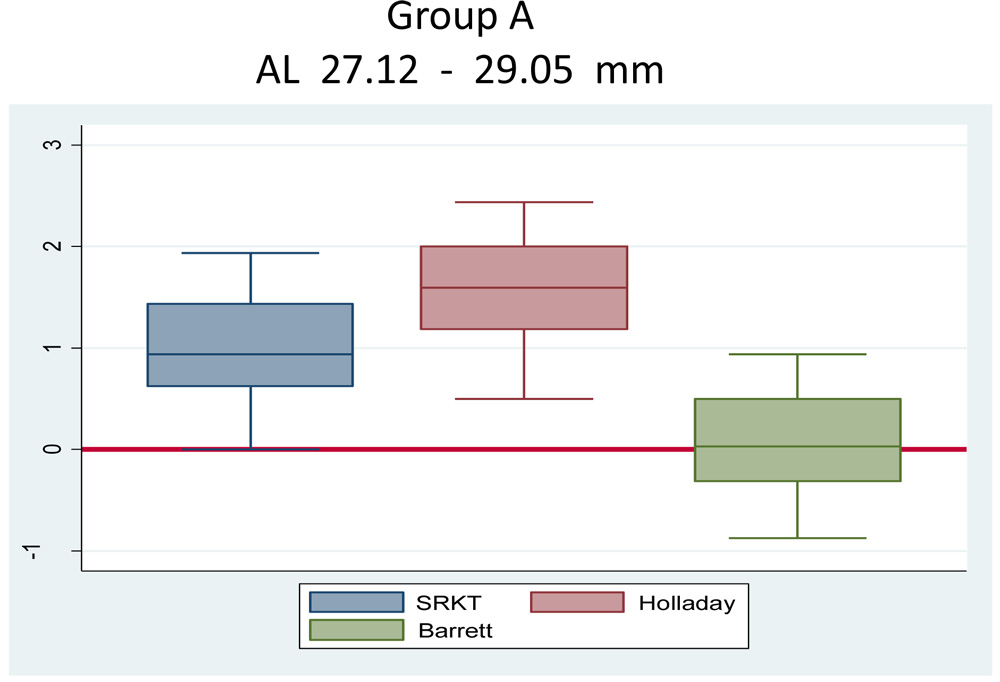
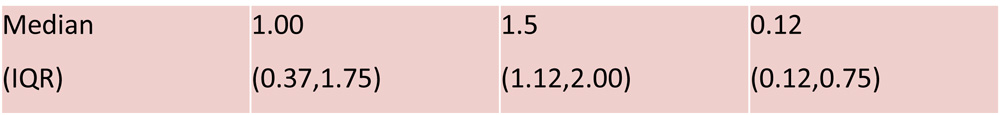
Group B
AL 29.14 – 31mm
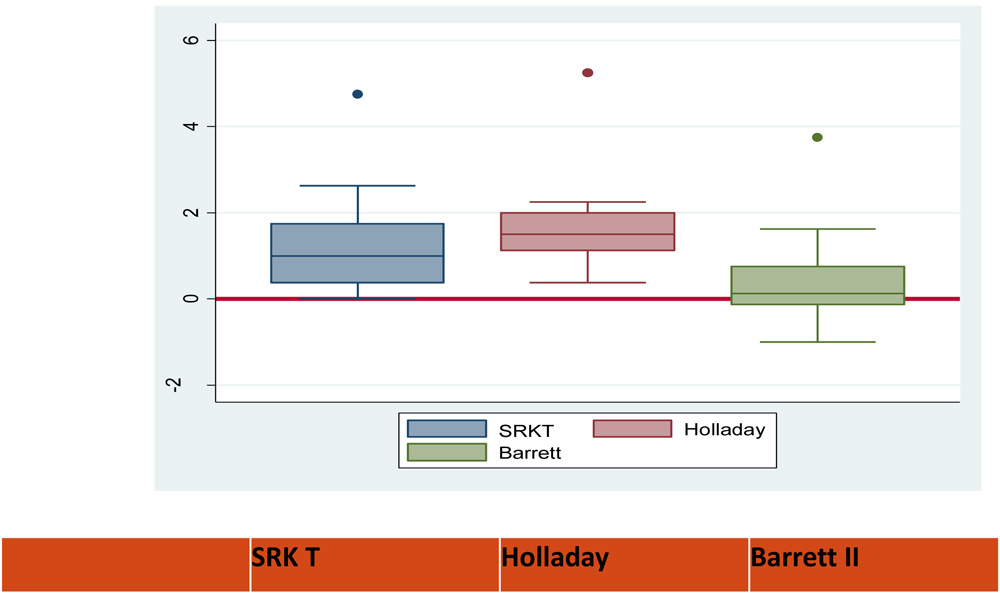

Group C
AL 31.56 – 33.22mm
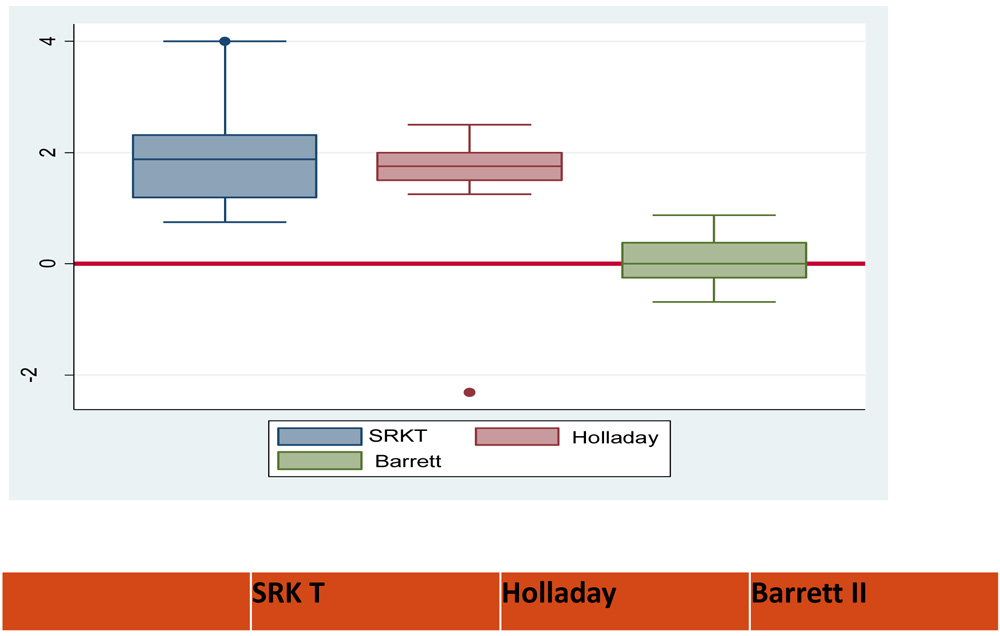
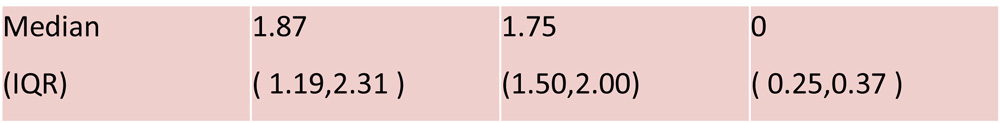
| Formulas | Group A
AL: 27.17-29.05 mm Median (IQR) |
Group B
AL:29.14-31 mm Median (IQR) |
Group C
AL: 31.56-33.22 mm Median (IQR) |
P value | |
| SRK-T | 0.94
(0.62-1.43) |
1.00
(0.37-1.75) |
1.87
(1.19-2.31) |
0.02 | |
| Hollday | 1.59
(1.19-2.00) |
1.50
(1.12-2.00) |
1.75
(1.5-2.00) |
0.68 | |
| Barrett II | 0.03
(0.31-0.50) |
0.12
(0.12-0.75) |
0
(0.25-0.37) |
0.54 | |
| P Value | < 0.05 | < 0.05 | < 0.05 |
Discussion
- In this study we found that theoretical IOL power calculated by Barrett II formula was closest to ideal IOL power.
- SRK T is doing well for calculation of IOL power of relatively lower AL but as AL increases it is not performing that well.
- Holladay is doing worst in all 3 groups.
- Barrett II is doing good in all 3 groups.
- Limitations – Small sample size
– Retrospective study .

