Dr.Mohammad Mehdi Raji, Dr. Alhaj F Tasneem, Dr.Nayak Vittal I, Dr. Md Sadegh Mirdehghan Farashah
Abstract:
Blepharoptosis is a common complaint of eyelid disorder. Frontalis suspension is a new method and the surgery of choice for congenital or acquired blepharoptosis with poor levator function (less than 4 mm). Autologous materials frequently used for frontalis suspension include fascia lata, temporalis fascia, and palmaris longus tendon. Synthetic materials used for frontalis suspension include polypropylene, monofilament nylon, polyfilament cable-type suture, polybutylate coated braided polyester, polyester fiber, expanded polytetrafloroethylene (ePTFE), and silicone. Each of these materials has its own advantages and disadvantages. Direct frontalis muscle flap procedure is a dynamic method of correction of severe ptosis, which is safe, effective, and stable with minimal complications and has great outcome over time, compared to traditional frontalis sling procedure.
Key Word: Blepharoptosis, Dynamic, Frontalis, Sling
Background:
Blepharoptosis is a common complaint of eyelid malposition in which the upper eyelid is lower than normal in primary gaze resulting in narrowing of the palpebral fissure.1This condition can cause both functional and cosmetic problems.Multiple surgical procedures are available including, simple skin excision, LPS resection, frontalis sling, levator advancement, Whitnall sling, frontalis muscle flap, and Mullerectomy. Selection of one technique over another depends on the several factors including the surgeon experience, the degree of ptosis, as well as the amount of levator muscle function.2 LPS action is measured by amount of lid excursion from extreme downward gaze to extreme upward gaze while negatingthe frontalis muscle action.Considerations, which helped to develop these surgical techniques, include the need for cosmetically acceptable results, preservation of the normal eyelid crease, maintenance of the normal tear film, and prevention of exposure keratopathy by prevention of over correction.3
Frontalis suspension is the surgery of choice for congenital or acquired blepharoptosis with poor levator function (less than 4 mm). Autologous materials frequently used for frontalis suspension include fascia lata, temporalis fascia, and palmarislongus tendon. Synthetic materials used for frontalis suspension include polypropylene, monofilament nylon, polyfilament cable-type suture, polybutylate coated braided polyester, polyester fiber, expandedpolytetrafloroethylene (ePTFE), and silicone.4Autogenous fascia lata remains the gold standard for frontalis suspension. Fascia lata has excellent tensile strength, lack of signifiant inflammatory response in surrounding tissues, and minimal risk for rejection, yet there are disadvantages, which include the need for a second operative site and increased surgical time. Also biointegration of fascia lata creates permanence, postoperative adjustment and removal is extremely difficult and harvesting in children under 3 years old is also difficult.4
Material & Methods:
A prospective study of 6 patients include 3 males and 3 females (8 eyelids) underwent suspension procedure of frontalis muscle flap overlapped with an inferiorly based orbital septum flap, between 2013 and 2015 in Ophthalmology Dept. of our hospital. All patients had severe blepharoptosis with poor LPS action. Patients age was in the range of 26 to 43 years old. Two patients had bilateral ptosis and four patients had unilateral ptosis. LPS action ranges from none to less than 4 mm.
Eyelid studies measurements were taken at baseline, 2 months and 6 months after surgery. The presence of complications, flap function and palpebral contour were evaluated.
Operation Method:
Frontalis Muscle Flap
In unilateral ptosis a lid crease is marked at a height symmetric with that of the opposite upper eyelid, while in bilateral ptosis, the lid crease is drawn 5 to 6 mm from the lash line.5
To control bleeding, local infiltration anesthesia of lidocaine HCL 2% with 1:100,000 epinephrine is infiltrated along the proposed incision line and nerve block anesthesia to the supraorbital foramen., to keep the movement of the frontalis muscle for observation during surgery.
In a plane between the orbicularis oculi muscle and the orbital septum, a careful submuscular dissection is performed superiorly. On the surface of the orbital septum, a trapezoidal flap on the superior border of tarsal plate is designed.
A suprabrow incision 1.5 to 2 cm superiorly along the margin of upper eyebrow is made about 2.5 cm in length. Injury to the supraorbital neurovascular bundle is avoided by starting the incision at least 5 mm lateral to the supraorbital notch.
The skin and subcutaneous structures are separated from the vertically oriented muscle fibers of underlying frontalis. The submuscular dissection is done till about 1.5 cm above the supraorbital margin of the frontal bone.
Two parallel cuts are made at the medial and lateral sides of the flap, forming a rectangular muscle flap. A tunnel is created above the orbital septum by passing blunt pointed scissors into the lid crease incision to emerge through the incision at the superior margin of the eyebrow.
The orbital septum flap is passed superiorly through tunnels and sutured to the anterior surface of the frontal muscle flap with three permanent 5-0 vicryl sutures through the central, medial, and lateral portions of the two flaps.
The skin is closed with running and interrupted nonabsorbable 6-0 sutures.
A temporary lid occlusive suture using a modified Frost suture is placed to protect the cornea and relieve tension on the sutures. This modified Frost suture is removed after 48 h. A pressure bandage is placed over the frontalis area to reduce the chance of hematoma formation.6
Results:
Ptosis was corrected in all 6 patients with good results in terms of functionality, contour and aesthetic outcome. (Fig.1)
All 8 eyes underwent ptosis correction had a symmetric redundant fold of preseptal skin according to the margin reflex distance-1 (MRD-1) measurement used to evaluate efficacy.
All the patients had incomplete closure of the eyelid for 3-4 months after the operation but experienced normal opening and closing of the palpebral fissure within 6 months. The suprabrow scar merged well with the eyebrows. The only complication was reduced eyelid excursion in extreme upward and downward gaze, which was mainly observed in the immediate postoperative period. Post operative forehead anesthesia was seen but totally recovered over a period of time. Complications such as eyebrow asymmetry, entropion, orbital hemorrhage and corneal exposure due to lagophthalmos were not seen in our series of patients. But probably we need to do more cases
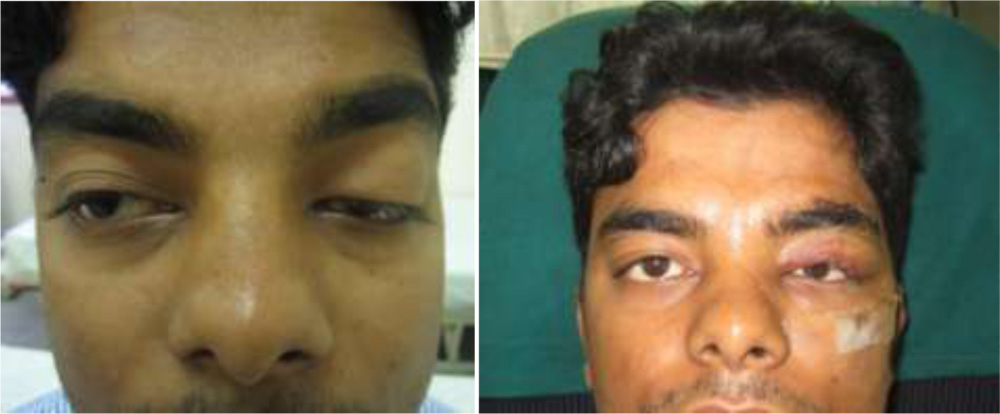 Figure 1: (Left) Preoperative appearance of a 28-year-old patient with left severeblepharoptosis
Figure 1: (Left) Preoperative appearance of a 28-year-old patient with left severeblepharoptosis
(Right) Postoperative day 1 appearance after suspension procedure of
frontalis muscle flap overlapped with an inferiorly based orbital septum flap
Discussion:
In patients having severe ptosis with levator function less than 4 mm two recommended procedures are traditional frontalis sling surgery and frontalis muscle flap procedure.
The frontalis sling procedure, is a static correction method of ptosis. In this procedure, the eyelid is surgically attached to the frontalis muscle at the desired height using autologous, heterologous or alloplastic material.
The frontalis muscle flap procedure is a dynamic correction method of ptosis which involves elevating the innervated frontalis muscle flap, passing it over a pulley created near the insertion of the orbital septum at the superior orbital rim, which redirects the pull of the frontalis to lift the lid, and then attaching the frontalis muscle to the tarsal plate. In this condition, the pulley lifts the eyelid towards eyebrow.7
The advantages of frontalis muscle flap procedure over the frontalis sling procedure include less lid lag on downward gaze, minimal ptosis on upward gaze, eyelid contour is maintained, reduced tendency for the eyelid to lift away from the globe with upward gaze, no risk of extrusion of sling materials and very low risk of ptosis recurrence. Additional advantage is that the procedure also can be performed on younger patients compare to traditional frontalis sling since the frontalis muscle is developed in first two years of life while fascia lata development may completed by three years of age.
Complications of frontalis muscle flap procedure include: (1) eyebrow asymmetry, (2) transient postoperative forehead anesthesia with spontaneous recovery, (3) reduced eyelid excursion in extreme upward and downward gaze, (4) lagophthalmos, and (5) overcorrection possibly because the frontalis muscle is stronger than the levator muscle.8,9
In this series, we have corrected cases of severe ptosis while avoiding injury to levator muscle of the upper eyelid by suspension of a frontalis muscle flap overlapped with an inferiorly based orbital septum flap, the dynamic frontal and levator muscles were connected by the orbital septum which an easy operation, relatively less traumatic, and a has better effect.
To observe frontalis muscle action during surgery, anesthesia to the frontalis muscle should be nerve block anesthesia of the supraorbital foramen.
No upward arching of the corrected eyelid margin occurs because the pulling force for elevating the lid is the normal direction of the levator muscle’s forces.
In unilateral ptosis cases, the position of the corrected lid margin should be 1 mm higher than the normal side. The frontalis muscle is a very powerful motor unit, and patients learn how to use it to keep the eyelid position at the proper functional and cosmetic position.
To prevent dehiscence of the suspending tissues, patients were informed not to lift the eyebrow or close the eye forcefully within 7 days postoperatively.
Conclusions:
Direct frontalis muscle flap procedure is a dynamic method of correction of severe ptosis, which is safe, effective, stable with better corneal protection and very less complications such as no ectropion, no risk of neurovascular injury and has great outcome over time, compared to traditional frontalis sling procedure.
References:
1. Sakol PJ, Mannor G, Massaro BM. Congenital and acquired blepharoptosis. Curr Opin Ophthalmol 1999;10:335-9.
2. Collin JRO (1990) The surgical management of ptosis. In: McCarthy JG (ed) Plastic Surgery. vol 2. 1st edn. Saunders, Philadelphia, 1759
3. Felicia D. Allard, Vikram D. Durairaj. Middle East African Journal of Ophthalmology, Volume 17, Number 2, April – June 2010
4. Cohen A.J, Weinberg D.A. Frontalis Suspension for the Correction of Blepharoptosis In: Evaluation and Management of Blepharoptosis, Springer Science+Business Media, LLC 2011
5. Callahan MA, Beard C (1990) Beard’s Ptosis. 4th edn. Aesculapius Publishing, Birmingham, AL
6. Pan Y., Zhang H., Yang L., Song B., Xiao B., Yi C. Correction of Congenital Severe Ptosis by Suspension of a Frontal Muscle Flap Overlapped with an Inferiorly Based Orbital Septum Flap, Aesth Plast Surg (2008) 32:604–612
7. Ramirez OM, Pena G. Frontalis muscle advancement: A dynamic structure for the treatment of severe congenital eyelid ptosis. Plast Reconstr Surg 2004;113:1841-9; discussion 1850-1.
8. Goldey SH, Baylis HI, Goldberg RA, Shorr N. Frontalis muscle flap advancement for correction of blepharoptosis. Ophthal PlastReconstr Surg 2000;16:83-93.
9. Islam ZU, Rehman HU, Khan MD. Frontalis muscle flap advancement for jaw-winking ptosis. Ophthal Plast ReconstrSurg 2002;18:365-9.

