Dr. Salil Kumar Mandal, M12531, Dr. Tamojit Chatterjee, Dr. Madhumita Banerjee
Dr.Salil Kumarc Mandal. Dr.Tamojit Chatterjee. Dr.Madhumita Banerjee
Abstract
Purpose; To evaluate the surgical and cosmetic outcomes and recurrence rates of the ocular malignancies with metastatic potentialafter lid/periosteum sparing orbital exenteration .
Methods; Prospective interventional case series of ten eyes and patients over a period of three years. All the patient had biopsy proved ocular malignancy with spreading tendency. Lid sparing orbital exenteration without removing periosteum was done in all the cases. Sockets and lid reconstruction were performed simultaneously. Patients were followed up for one year.
Results; All the ten patients had satisfactory post surgical, cosmetic and functional outcomes. Preserving periosteum in the orbit is very effective for split thickness skin graft to accept on host and helps in successful lid reconstruction from forehead rotational flap.
Conclusion; Lid sparing orbital exenteration without removing periosteum is effective for socket reconstruction with split thickness skin graft. No recurrence of malignancy was noted in one year follow up period.
Introduction: Orbital exenteration is commonly done in cases of malignant neoplasm of the orbital content either primary or secondary spread from adjacent structure which are not treatablewith simple excision and radiotherapy. Orbital exenteration is classified as total,subtotal and super exenteration. According to Levin et.al indications for orbital exenteration are as follows-
1. Life threatening malignancy
2.Life threatening infection
3.Intractable pain and deformity
In this study all the ten cases were done for malignancy with life threatening situation. Lid sparing orbital exenteration with retention the of orbital periosteum along withSplit thickness skin grafting to cover orbital periosteum and fore head rotational flap was performed for lid reconstruction followed by fitting of prosthesis to bring an acceptable cosmetic outcome
AIMS AND OBJECTIVES
To evaluate the surgical and cosmetic out come
To evaluate the recurrence of the ocular malignancy with spreading tendency after lid sparing orbital exenteration .
To evaluate effectiveness of socket and lid reconstruction without removing periosteum and prosthetic fittings
Methods;
Prospective interventional case series of ten eyes and patients over a period of three years. All the patient had biopsy proved ocular malignancy with spreading tendency.In this study 5 patient were female and 3 patient were male . Lid sparing orbital exenteration without removing periosteum done in all the cases. Split thickness skin grafting done to cover the orbital bone. Sockets and lid reconstruction performed simultaneously followed by prosthetic fitting. Patients were followed up for one year.
Inclusion criteria
1.Malignancy strictly confined to orbital content without invading the periosteum
2.Malignancy invading the lid margin upto 2-3 mm.
3.No h/o chemotherapy and radiotherapy
4.Regional lymph node biopsy negative
Exclusion criteria
1.Malignancy spreading to adjacent structures invading the periosteum
2.Distant metastasis
3.Regional lymph node biopsy positive cases.
4.H/o chemotherapy and radiotherapy.
In this study males were 4 and females were 6 in number.In this study age ranges from 45 to 80.In this study squamous cell ca were 6 basal cell ca 2 orbital meningeal mesothelial tumor 2.
Surgical procedure: Incision line is marked first. Surgical incision made 8-9 mm away from lid margin directly reach to the orbital margin. Orbital septum exposed but not disturbed .Over the periosteum all the soft tissue including optic nerve with eye ball is removed. Spit thickness skin grafting made over periosteum of the orbital bone.Fore head rotation flap made with eye palpebral aperture fixed with cut margin of the sparing lid. Follow up ranges from one years to 2years
Clinical Data of the Seven Cases
| No | Age | Sex | Tissue of orgin | H.P | Type of Operation | Post Of Rt | Post of CT | Live/Death |
| 1 | 70 | f | Conjunctiva Cornea Lid | Squamous cell Ca | LidSparing Exenteration with lid reconstruction | no | NO | Live 3yrs |
| 2. | 74 | f | Ocular surface + lid | Squamous cell Ca | LidSparing Exenteration with lid reconstruction | no | no | Live 2yrs |
| 3 | 45 | f | Optic nerve sheath | Meningeal mesothelioma | LidSparing Exenteration | no | no | Live2.5yrs |
| 4 | 60 | M | Optic nerve sheath | Meningeal mesothelioma | LidSparing Exenteration | NO | NO | Live3yrs |
| 5. | 78 | f | Conjunctiva Cornea Lid | Squamous cell Ca | LidSparing Exenteration | no | no | Live2yrs |
| 6 | 64 | M | Conjunctiva Cornea Lid | Sebeceous cell ca | LidSparing Exenteration with lid reconstruction | no | no | Live 1.5yrs |
| 7. | 65 | M | Conjuctiva involving lid | Squamous cell ca | LidSparing Exenteration with lid reconstruction | no | no | live2yrs |
| 8. | 68 | M | Lid | BCC | LidSparing Exenteration with lid reconstruction | no | no | Live 2.5 |
| 9 | 56 | F | Lid conjunctiva | BCC | LidSparing Exenteration with lid reconstruction | no | no | Live 3yrs |
Results and observation;Total no of patients were ten of which males were 4 and females were 6.Lid sparing orbital exenteration with retaining the orbital periosteum simultaneously performing forehead rotational flap for lid reconstruction was done in all the cases. All the patient were followed up for one year .No recurrence of the disease was observed during the followup period.All the patients had moderate to good cosmetic outcomes with adequate prosthetic fittings . Most cases were categorized as orbital, ocular, and adnexal malignancy, with squamous cell ca (6) and basal cell carcinoma(2) being the most common.Complications occurred in some of the cases. Infection and partial graft rejection was the commonest .It was treated conservatively with systemic antibiotic and anti inflammatory drugs. In this study all patient retained prosthesis for good cosmesis throughout the post operative period .H.P.E report of all patients had margin free tumor margins .None of the case had involvement of the optic nerve. During the follow up period none of the patients died due to recurrence of the disease.
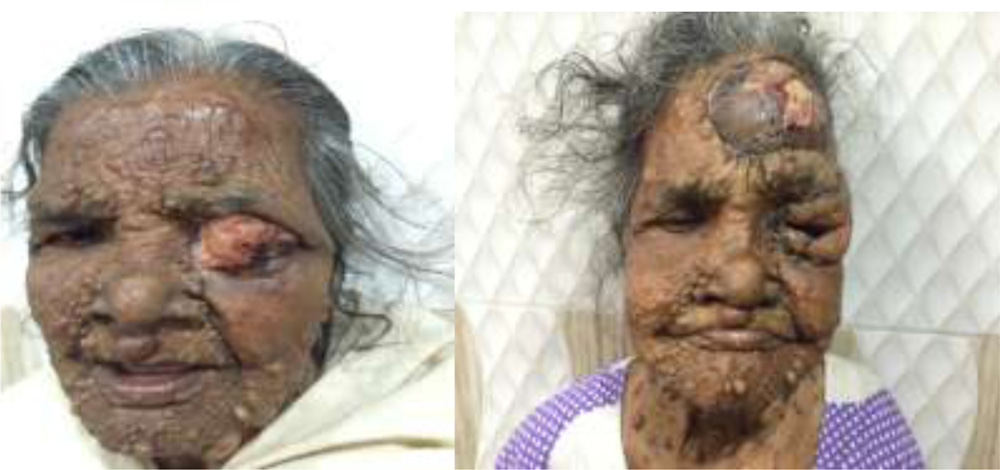
Fig -1 Preoperative and post operative image of lid sparing orbital exenteration.with forehead rotational flap for lid reconstruction
Discussion ; Orbital exenteration is highly disfiguring surgery. It is to be done as life saving, desperate procedure. It may cause complete removal with success in cases of locally invasive tumor e.g squamus cell ca. basal cell ca and meningeal mesothelioma. Orbital exenteration with tumor free margin helps in long term follow up with no recurrence and no such death results in this study. Squamous cell carcinoma was the most prevalent in our series. This is slightly different than the series described by Rathbun and associates. In contrast they found 30% of the cases (14/48) to be basal cell carcinoma, and only 12.5% (6/48) to be Squamous cell carcinoma. Squamous cell ca is more aggressive than the basal cell ca and it requires more extensive surgery because of perineural involvement. Several authors thought about disfiguring effect of the surgery that is why lid sparing orbital exenteration is chosen for this study.It may cause rapid healing with good cosmetic outcomes. Shields and associates report that eyelid sparing technique can be used in most of the cases of malignant tumors and in more than half of the cases originating in the eyelids In this study all the cases underwent lid sparing orbital exenteration with preserving periosteum for split thickness skin graft
In this study we preserved the orbital tissue as much as possible. After removal of the tumor routine map biopsies were taken from various parts of the orbit . One must take into consideration the biological behavior of the tumor. In cases of highly malignant infiltrative tumors such as adenoid cystic carcinoma of the lacrimal gland or conjunctival malignant melanoma, which are potentially surgically curable we prefer a wider surgical margin and additional separate intraorbital map biopsies after removing the tumor en-bloc. If surgical cure is not possible
then limited debulking is performed. Most important part of the patient rehabilitation is the lid reconstruction in exenterated eye. In this study we prefer exenteration with preserving orbital periosteum for split thickness graft. In bare bone split thickness skin graft is not accepted properly .That is why we prefer periosteum to be retained in all the cases. thehead rotational flap is mounted over the lid sparing part for lid reconstruction .This will help in retaining the prosthesis with proper support for a longer period. Subtotal exenteration with preservation of orbital tissue volume, eyelids, or conjunctiva may facilitate the use of orbital and ocular prosthesis and improve esthetic and functional out come. Regarding the complication in this series infection and partial graft rejection were the most common. One case had fistulae formation another two cases had displacement of the prosthesis .This is treated with simple tract excision and conservative management by systemic antibiotics. Interestingly, Yassur and associates report the efficacy of becaplermin gel (recombinant human platelet derived growth factor) for the treatment of chronic orbital ulcer after exenteration. Orbital exenteration is successful in the surgical treatment of squamous cell ca and basal cell ca. Success rate of the surgery depends upon the tumor free margin before metastasis to the distant organs. In this study all case done with wider tumor free margin with no optic nerve involvement .If the tumor margin is very close chemotherapy and radiotherapy increases the life span of the patient. Aesthetic reconstruction of the exenterated orbit is complicated but may be associated with good cosmetic results. It is more likely to be successful in cases of subtotal exenteration . The best functional and cosmetic outcome are judged by the ability to wear a prosthetic device, the absence of a patch, and the lack of postoperative complications such as sino-orbital fistula.
Conclusion; Lid sparing orbital exenteration with preservation the orbital periosteum for split thickness skin graft followed by forehead rotational flap for lid reconstruction is effective for prosthetic fit without patch .It is functionally, anatomically and cosmetically more effective in long term follow up period. Patients psychological status is also much more satisfactory.
REFERENCES
- Rathbun J, Beard C, Quickert MH. Evaluation of 48 cases oforbital exenteration. Am J Ophthalmol 1971;30:191–199.
- Pushker N, Kashyap S, Balasubramanya R, et al. Pattern oforbital exenteration in a tertiary eye care centre in India.Clin Experiment Ophthalmology 2004;32:51–54
- Mauriello J Jr., Han KH, Wolfe R. Use of autogenously split-thickness dermal graft for reconstruction of the lining ofthe exenterated orbit. Am J Ophthalmol 1985;100:465– 467.Putterman A. Orbital exenteration with spontaneous granulation.Arch Ophthalmol 1986;104:139 –140.
- Reese A. Exenteration of the orbit with transplantation ofthe temporalis muscle. Am J Ophthalmol 1958;45:386 –390.
- Reese A, Jones IS. Exenteration of the orbit and repair bytransplantation of the temporalis muscle. Am J Ophthalmol1961;51:217–227.
- Cuesta-Gil M, Concejo C, Acero J, Navarro-Vila C, OchandianoS. Repair of large orbito-cutaneous defects by combiningtwo classical flaps. J Craniomaxillofac Surg 2004;32:21–27.
- Menon N, Girotto JA, Goldberg NH, Silverman RP. Orbitalreconstruction after exenteration: use of a transorbital temporalmuscle flap. Ann Plast Surg 2003;50:38–42.
- Wax M, Burkey, BB, Bascom D, Rosenthal EL. The role offree tissue transfer in the reconstruction of massive neglectedskin cancers of the head and neck. Arch Facial Plast Surg2003;5:479–482.
- Uusitalo M, Ibarra M, Fulton L, et al. Reconstruction withrectus abdominis myocutaneous free flap after orbital exenterationin children. Arch Ophthalmol 2001;119:1705–1709.
- Bartley G, Kasperbauer JL. Use of a flap of extraocular muscleand fat during subtotal exenteration to repair bony orbitaldefects. Am J Ophthalmol 2002;134:787–788.
- Lee H, Hong JP, Kim KT, Chung YK, Tark KC, Bong JP.Orbital floor and infraorbital rim reconstruction after totalmaxillectomy using a vascularized calvarial bone flap. PlastReconstr Surg 1999;104:646–653.
- Lim N, Mulhern MG, Joshi N, Waterhouse N, Peterson D,Coghlan B. The use of autologous autoclaved bone in orbitalreconstruction after exenteration for invasive cutaneouscarcinoma. Orbit 2002;21:181–187.
- Nerad J, Carter KD, LaVelle WE, Fyler A, Branemark PI.The osseointegration technique for the rehabilitation of theexenterated orbit. Arch Ophthalmol 1991;109:1032–1038.
- Sevel D. Exenteration of the orbit using a frontal periostealflap. Head Neck Surg 1981;4:154 –160.
- Goldberg R, Kim JW, Shorr N. Orbital exenteration: resultsof an individualized approach. Ophthal Plast Reconstr Surg2003;19:229 –236.Malhotra R, Chen C, Huilgol SC, Hill DC, Selva D.Mapped serial excision for periocular lentigo maligna and
- 16lentigo maligna melanoma. Ophthalmology 2004;110:2011–2018.
- McKelvie P, Daniell M, McNab A, Loughnan M, SantamariaJD. Squamous cell carcinoma of the conjunctiva: a series of26 cases. Br J Ophthalmol 2002;86:168 –173.
- Cook B, Bartley GB. Treatment options and future prospects for the management of eyelid malignancies. Ophthalmology2004;108:2088 –2098.
- Shields J, Shields CL, Demirci H, Honavar SG, Singh AD.Experience with eyelid-sparing orbital exenteration: the2000 Tullos O. Coston Lecture. Ophthal Plast Reconstr Surg2001;17:355–361.
- Catalano P, Laidlaw D, Sen C. Globe sparing orbital exenteration.Otolaryngol Head Neck Surg 2001;125:379 –384.

