Dr.Lional Raj D, L16453
Purpose
To evaluate the clinical outcomes of Pre Descemets Endothelial Keratoplasty (PDEK) in varied endothelial dysfunctions and to compare with conventional procedures of Penetrating Keratoplasty (PK) ,Descemets Membrane Endothelial Keratoplasty (DMEK) and Descemets Stripping Endothelial Keratoplasty (DSEK) in our practice.
Study Design
Prospective observational case series of clinical outcomes of PDEK and Quality of life (QOL) evaluation over the period of last two years done at Dr.Agarwal’s Eye Hospital Tirunelveli ,South India.IRB approval, Informed surgical consent were obtained.
Materials and Methods
Cases of varied endothelial dysfunctions namely Fuchs dystrophy, bullous keratopathies, failed corneal grafts, ICE and Pseudoexfoliation syndromes, post-hydrops corneas and post trabeculectomy glaucoma with endothelial dysfunctions were enrolled. {n=48}
Surgical technique
The donor endothelial side was placed up and a26 gauge needle attached to a 5ml air-filled syringe, a pneumatic dissection of pre-Descemets layer was created with a single bubble and stained with Tryphan blue. A 7.5- 8mm donor tissue (PDEK graft) was excised and implanted through medicel (MIL) injector, after conventional Descemets stripping of recipient cornea. The graft was then unrolled and attached to the recipient cornea with air injection and endo illuminator assistance (which would be video presented).
Results
48 subjects were enrolled.
Mean followup was 6 Months +/- 21 Days.
39 subjects(81.25%) achieved postoperative vision 20/60 or better.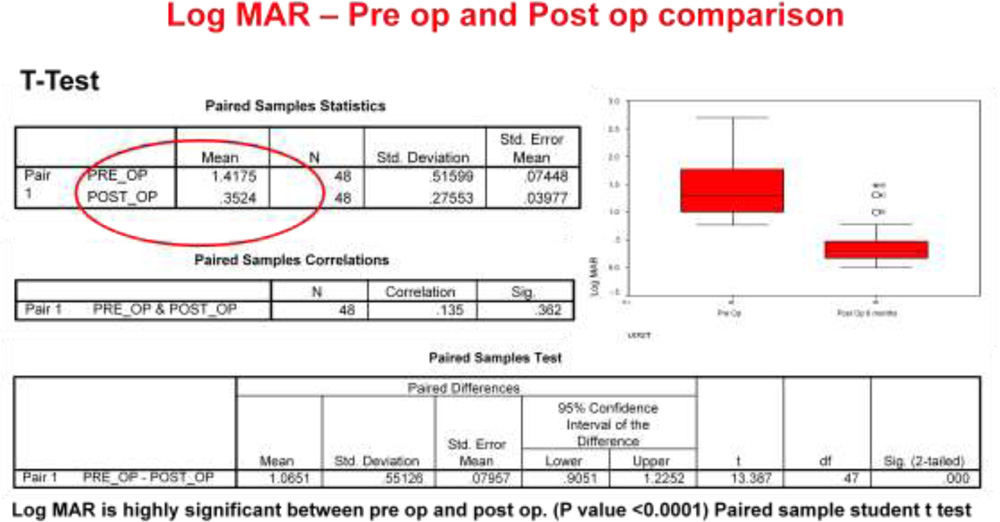
PDEK graft is possible in donor of any age against 40 years with DMEK.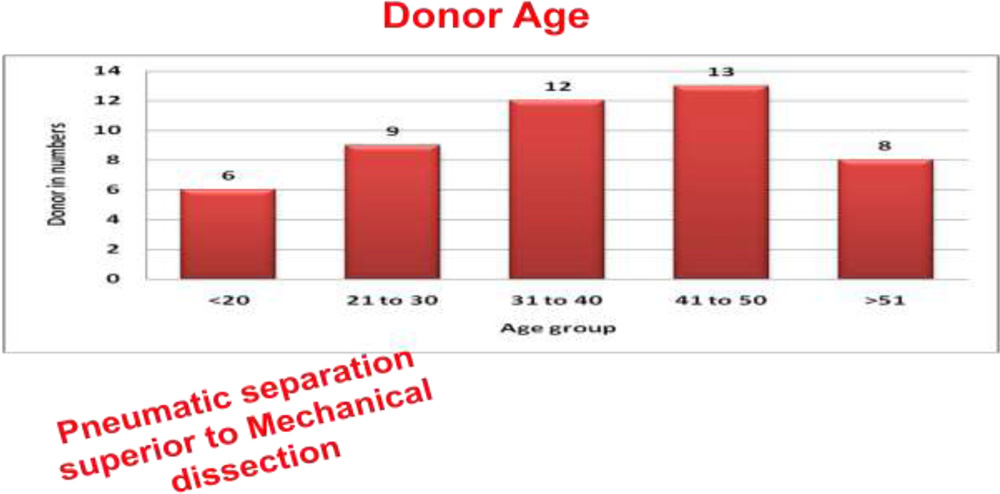
The mean surgical time was 43 minutes in PDEK, significantly lower than DMEK (approximately 90 minutes).
Endothelial preservation with PDEK (pneumatic dissection) was better than DMEK (manual dissection).
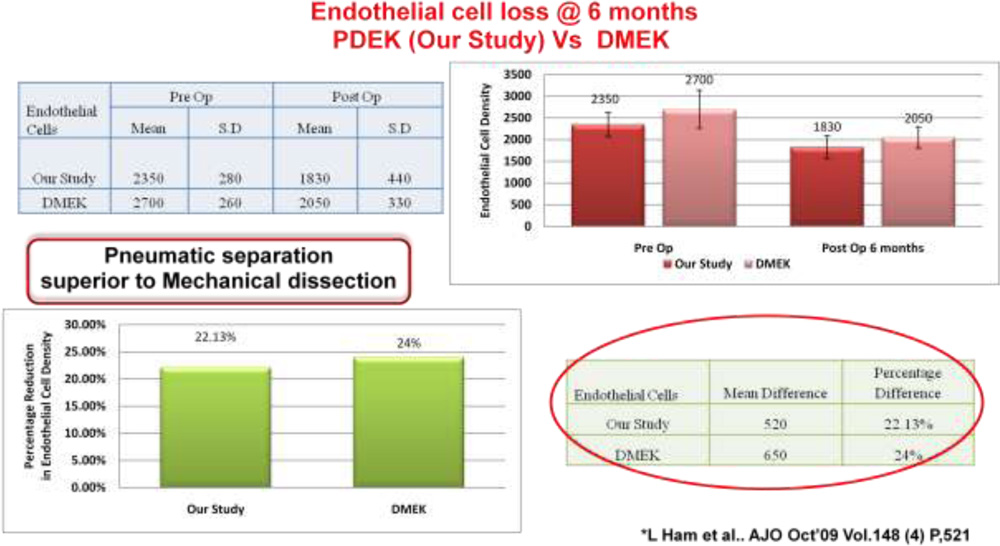
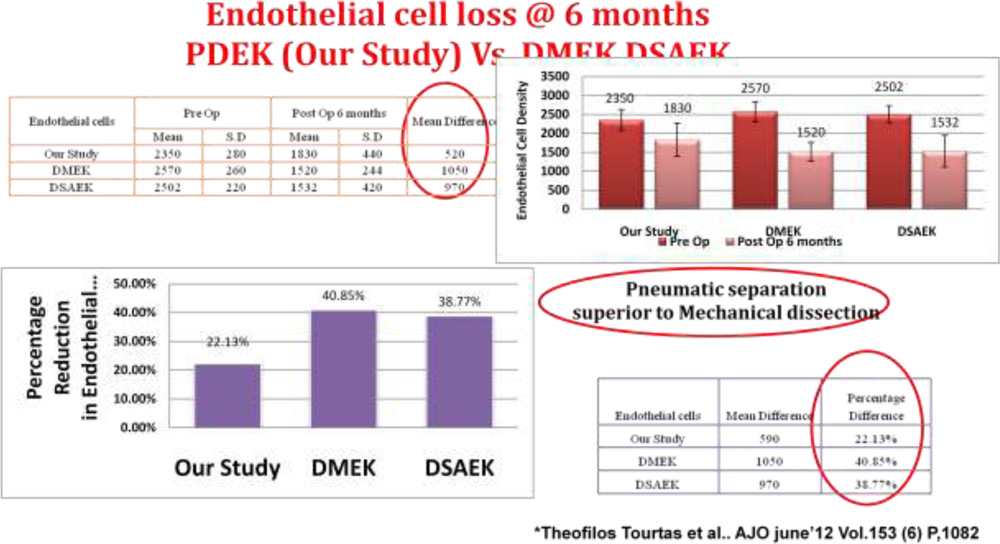
Corneal thickness of PDEK was closer to normal and DMEK against DSEK wherein corneal thickness was more

Quality of life in PDEK, a day care procedure had better pain and recovery scores than penetrating keratoplasties (7-10 days in PDEK Vs 6-12 months in PK).
No suture emergent adverse events with PDEK unlike PK
Conclusion
Pneumatic dissection of PDEK graft was technically easier, better in endothelial preservation and could be done in donors of any age when compared to manual dissection of DMEK.
Corneal thickness was closer to normal with PDEK than DSEK.
QOL assessment with PDEK was definitely better than PK in terms of pain, recovery,quality of vision and negligible suture related adverse events.
PDEK (Pre Descemets Endothelial Keratoplasty) is our preferred endothelial keratoplasty of choice and endoilluminator is an essential part of our procedures.

