Dr.Namitha Rachel Mathew, Dr. Sulatha V Bhandary.Dr. Krishna Addoor Rao, Dr. Divya Handa, Dr.Rudhira M Reddy
PRESENTING AUTHOR- DR NAMITHA RACHEL MATHEW
CHIEF AUTHOR- DR SULATHA V. BHANDARY
Introduction
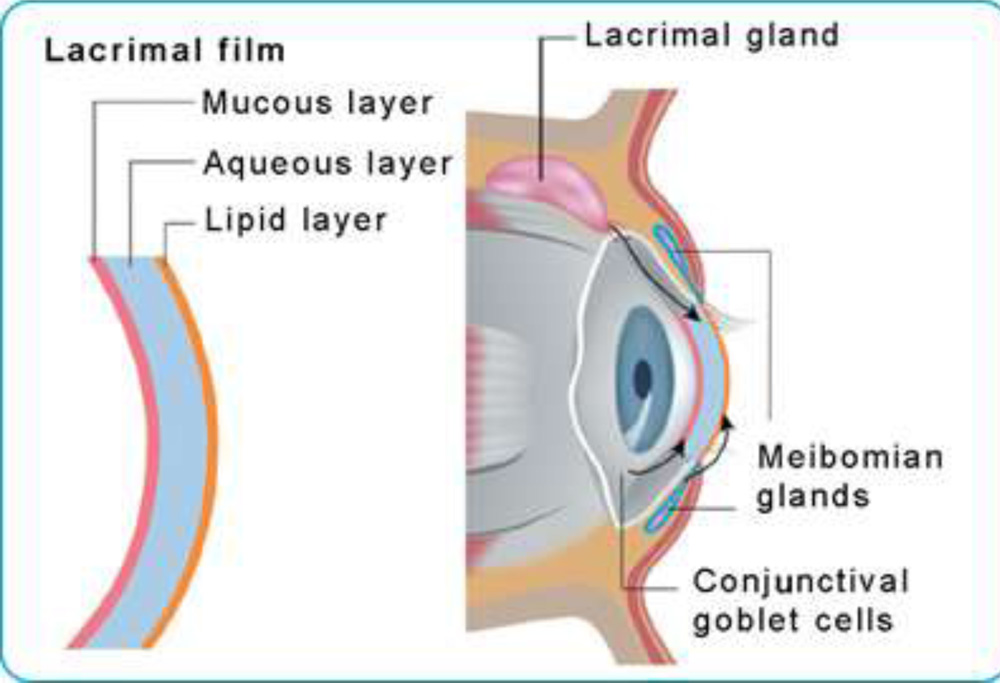
Dry eye is a heterogenous, multifactorial disorder of the preoculartearfilm – a common but under-diagnosed condition in Ophthalmology.
The tear film has three layers:
- Lipid layer secreted by the meibomian glands
- Aqueous layer secreted by the lacrimal glands
- Mucous layer secreted by conjunctival goblet cells.
Examination methods–
- SLIT LAMP EVALUATION
Of meibomian gland orifices & lid margin anatomy
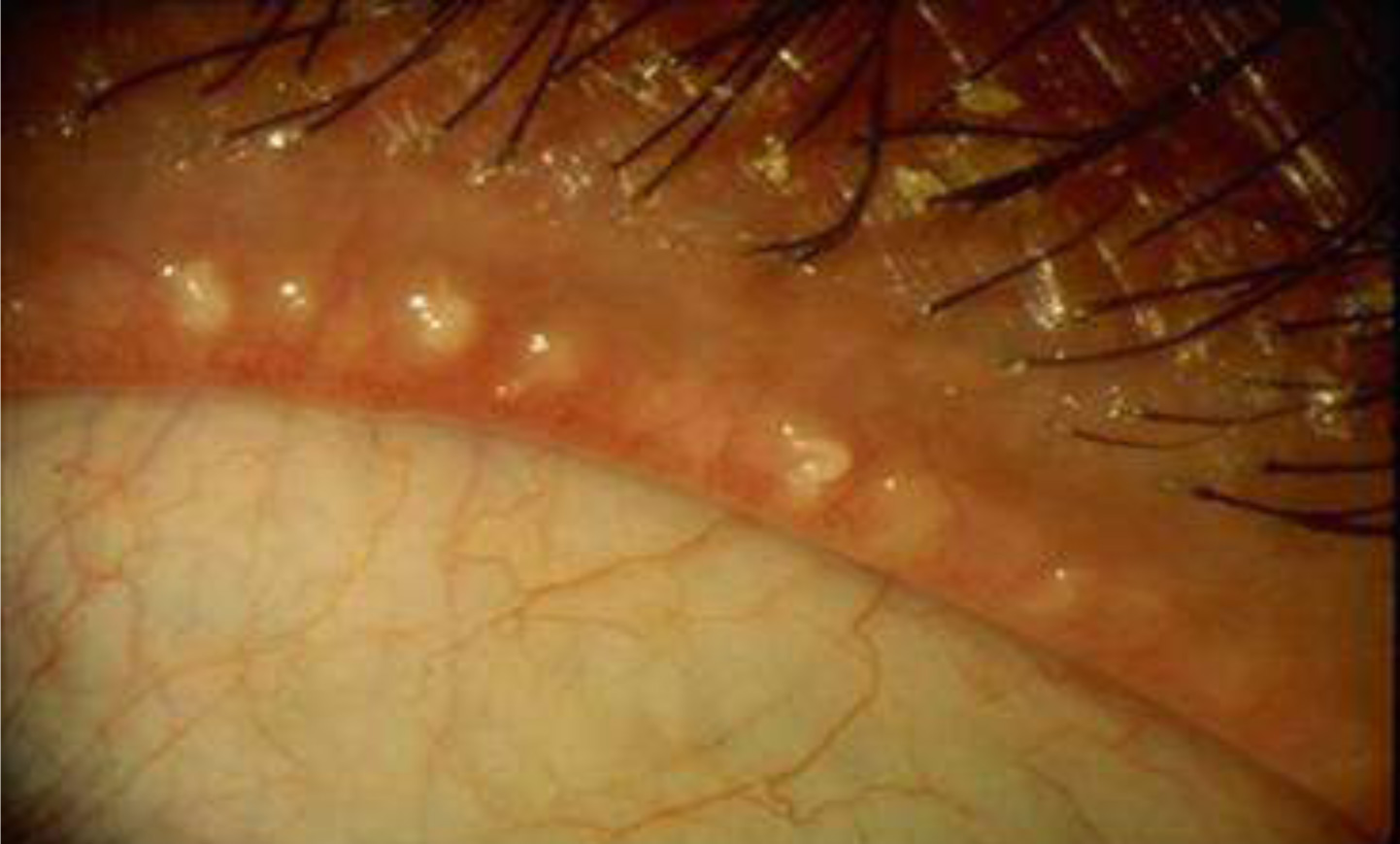
- MEIBOMETRY
Measures lipid secretion by the glands
- MEIBOGRAPHY
Images the meibomian glands with infrared light.
The prevalence of dry eye is difficult to estimate. It ranges between 7.8% in the western world to 93.2% in Asia.
This is probably because of two reasons-: the geographical location of the study population and the lack of standardization of the selected population, dry eye questionnaires, objective tests and dry eye diagnostic criteria.
AIM–
- To evaluate meibomian gland dysfunction (MGD) using non-contact infrared meibography in subjects with dry eye
- To analyze patients with positive MGD & normal Schirmer’s test & vice versa.
MATERIALS AND METHODS–
- A case control study
- Duration- 2 years
Sample size – 60 cases with dry eye symptoms & 60 controls.
The following tests were performed on all subjects-
- Ocular Surface Disease Index (OSDI) questionnaire
- Tearfilm Break Up Time (TBUT)
- Schirmer’s test
- Noncontact Infrared Meibography
RESULTS–
- OSDI–
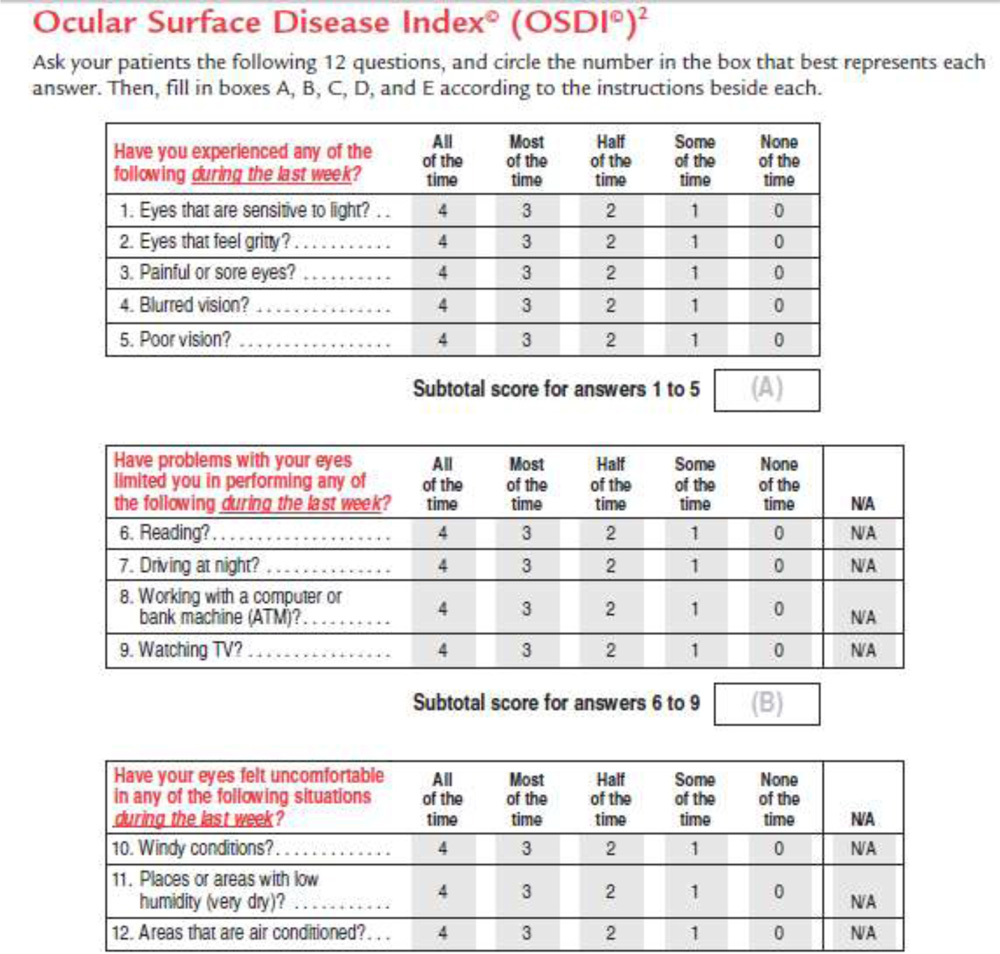
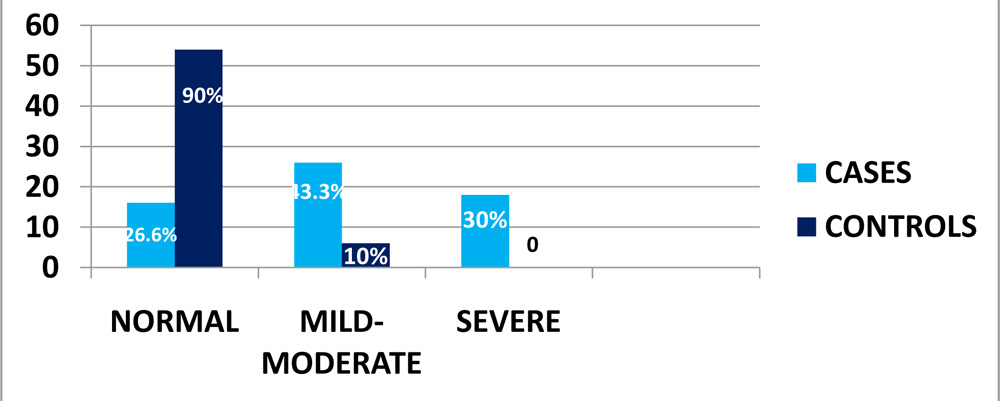 The OSDI questionnaire picked up dry eye subjects with a statistically significant p<0.0001
The OSDI questionnaire picked up dry eye subjects with a statistically significant p<0.0001
- SCHIRMER’S TEST-
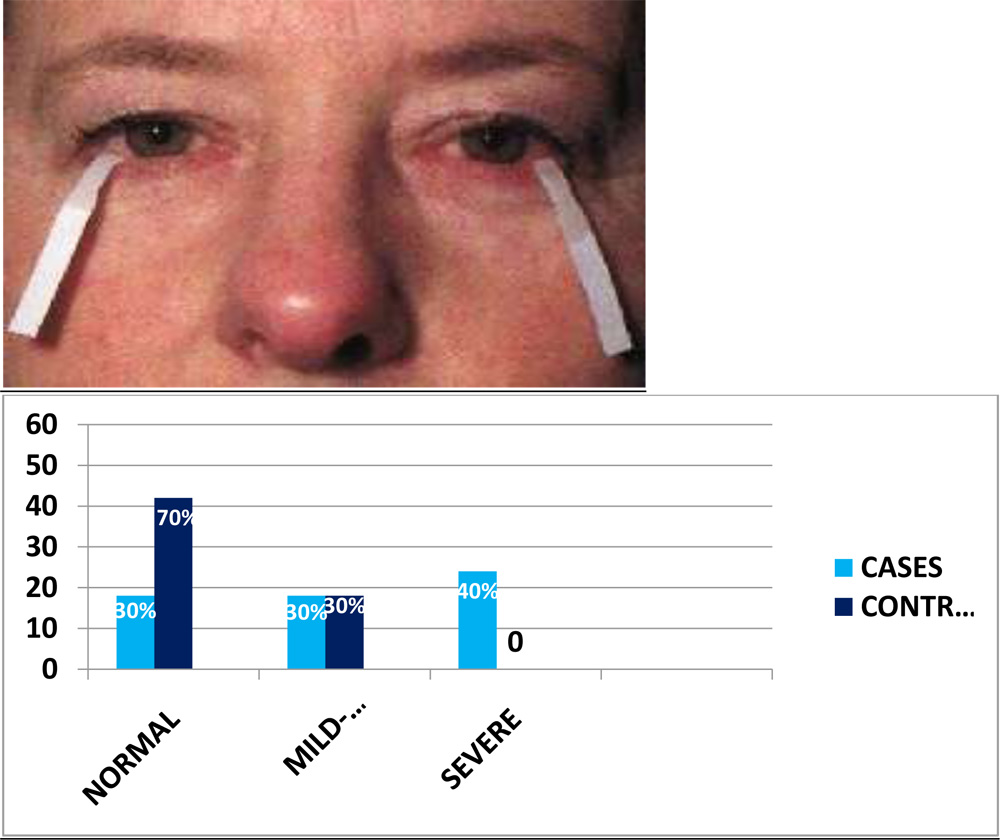
Schirmer’s test picked up dry eye subjects with a statistically significant p<0.0001.
- TEARFILM BREAKUP TIME–
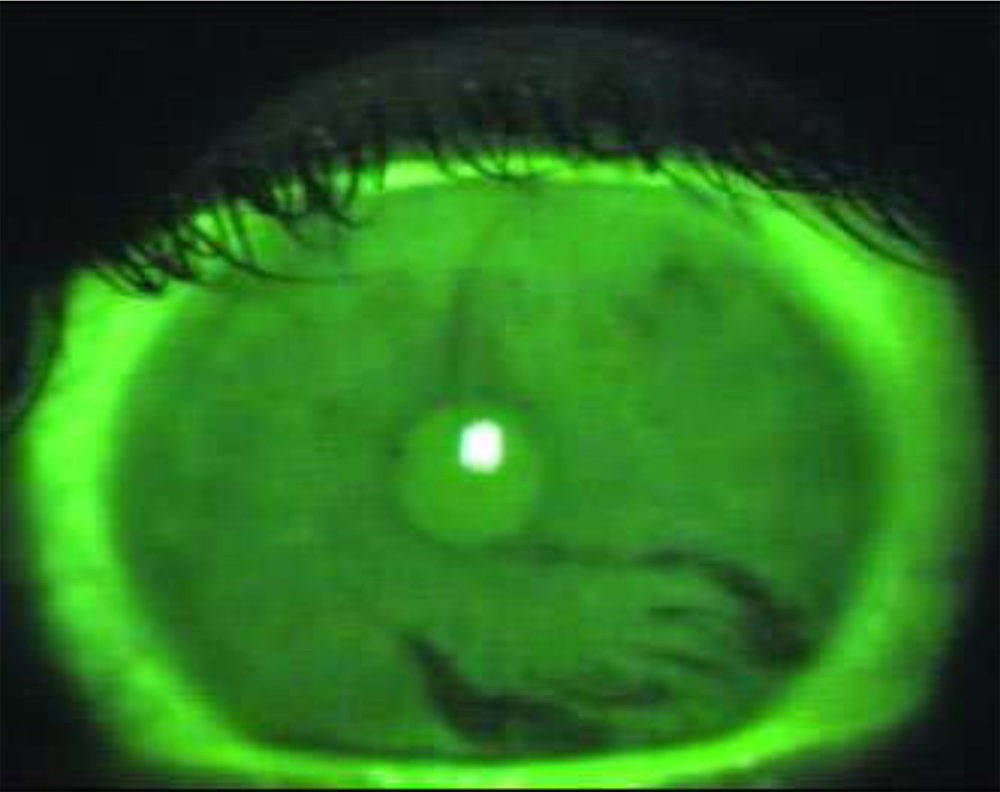
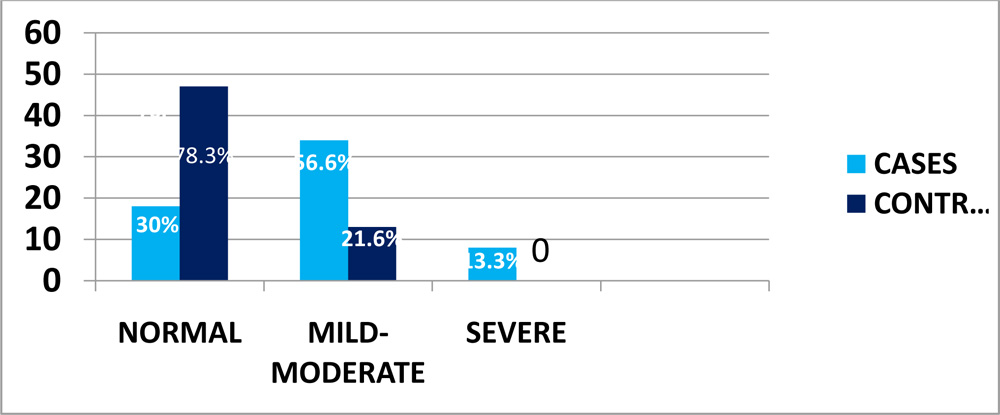
TBUT picked up significant number of dry eye subjects with a p<0.0001.
- MEIBOGRAPHY–
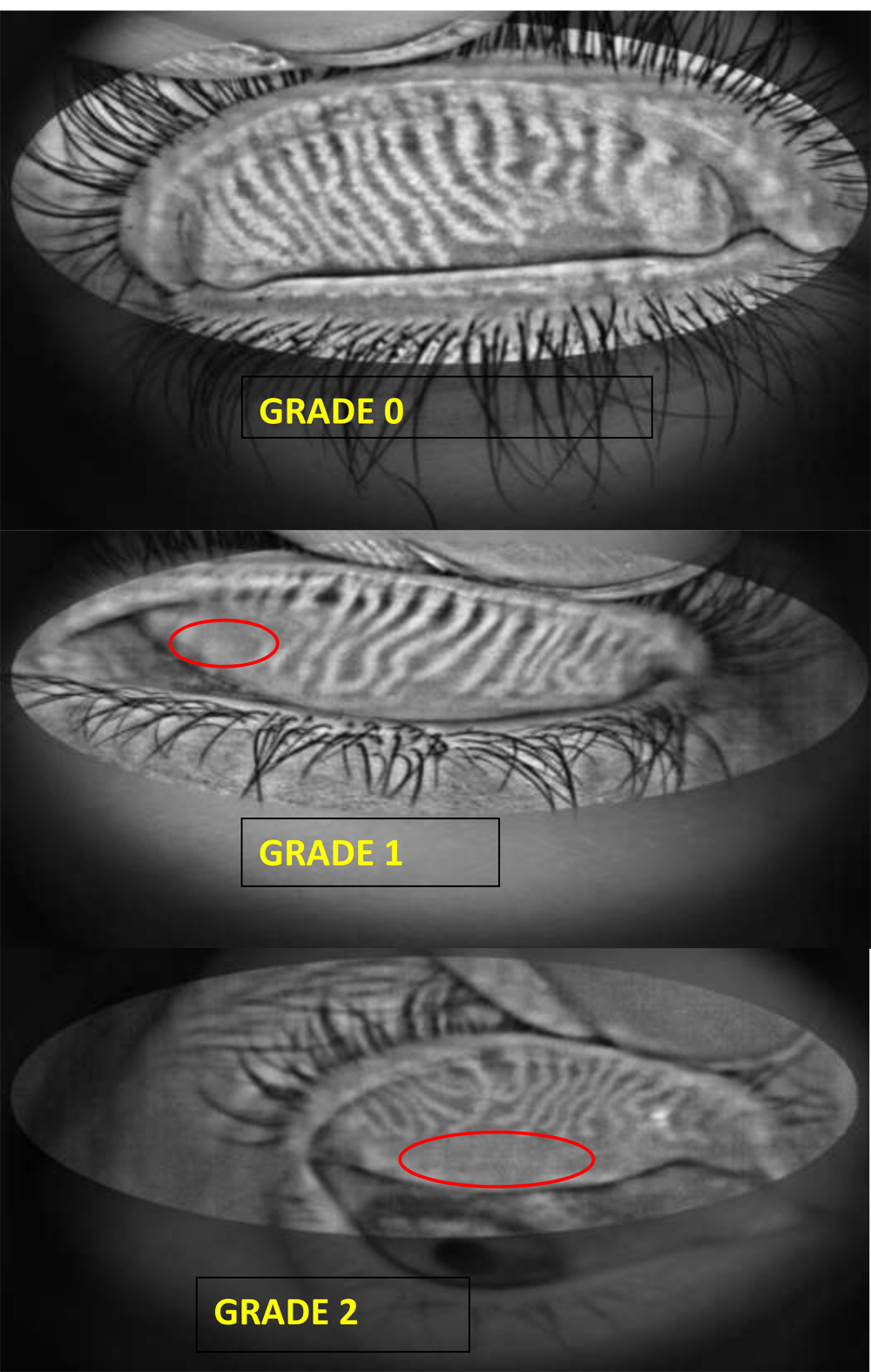
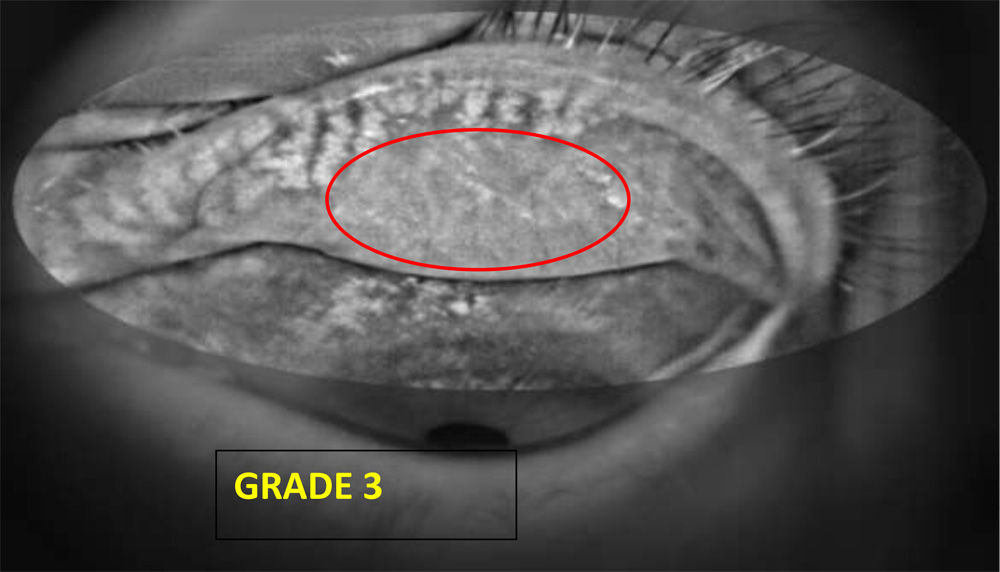
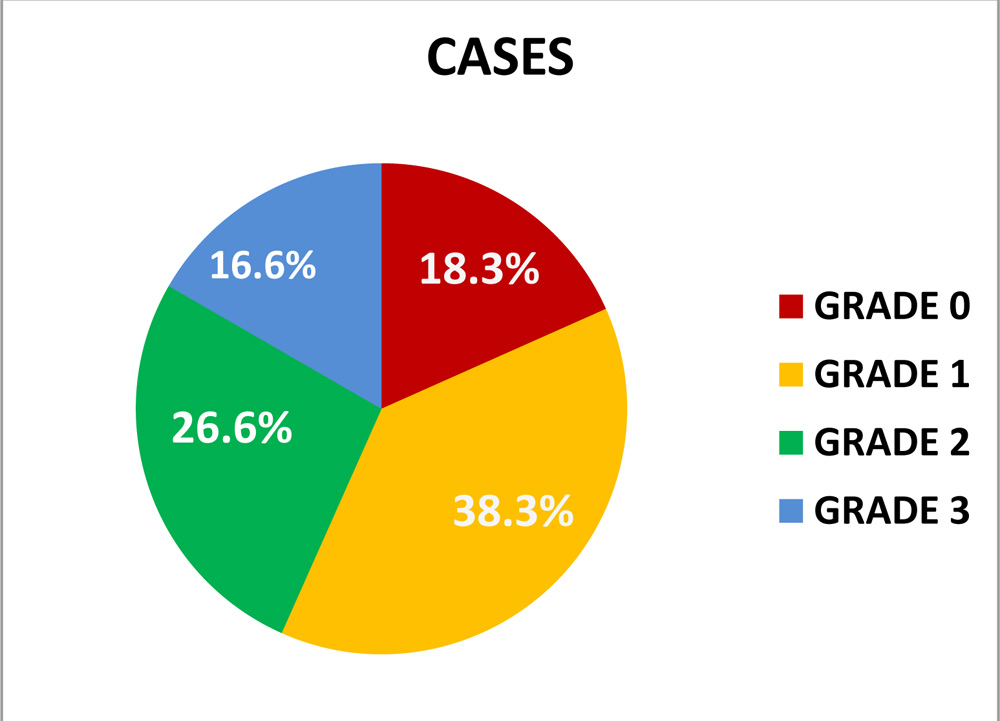
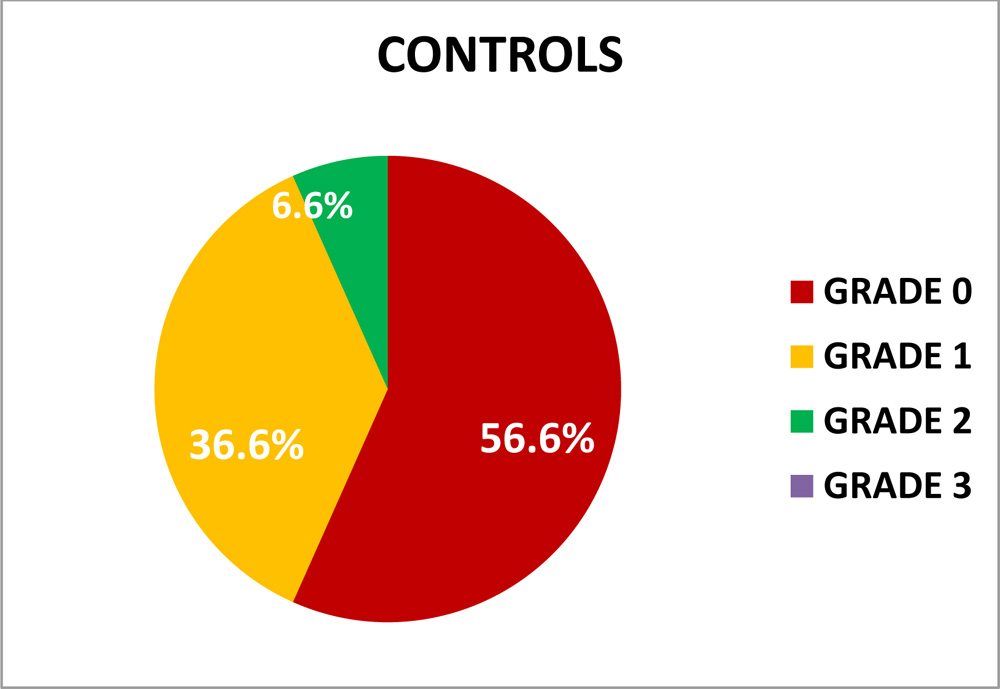
Meibography picked up many subjects with meibomian gland dysfunction among both cases and controls, which were further graded from grades 1-3, based on severity of meibomian gland dropout, and we obtained a p=0.004.
CONCLUSION-
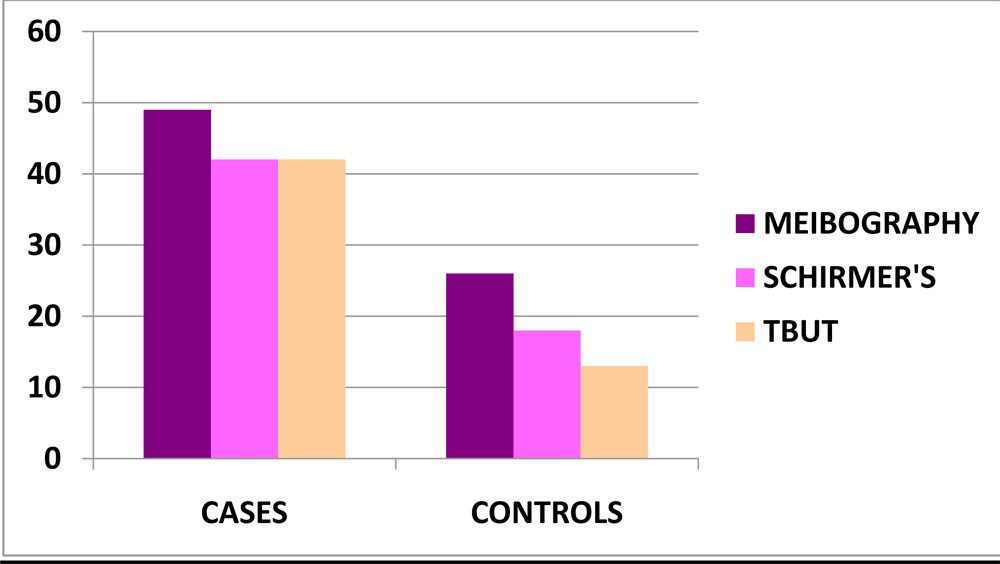 Among 60 cases, meibography picked up 7 dry eye subjects more than both schirmer’s and TBUT.
Among 60 cases, meibography picked up 7 dry eye subjects more than both schirmer’s and TBUT.
Among 60 controls, meibography picked up 8 dry eye subjects more than schirmer’s and 13 more than TBUT.
To conclude, non- contact infrared Meibography is superior to the conventional dry eye tests like tearfilm break up time and Schirmer’s test in picking up dry eye subjects. Moreover, it is non-invasive and more specific for meibomian gland dysfunction.
References–
- Matalia H, Ranganath A, Meda DR, Parekh R. Study of non-contact infrared meibography and non-invasive tear film break up time in normal and evaporative dry eye subjects. ESCRS 2014
- Wise RJ, SobelRK,Allen RC. Meibography: A review of techniques and technologies. Saudi J Ophthalmol. 2012 October; 26(4): 349–356
- Alsuhaibani AH, Carter KD, Abràmoff MD, Nerad JA. Utility of meibography in the evaluation of meibomian glands morphology in normal and diseased eyelids. Saudi Journal of Ophthalmology Volume 25, Issue 1, January–March 2011, Pages 61–66
- Arita R. Itoh K. Inoue K. Amano S. Noncontact Infrared Meibography to Document Age-Related Changes of the Meibomian Glands in a Normal Population. May 2008Volume 115, Issue 5, Pages 911–915
Comment-incomplete foormat. No mentuon of consent statistical methods comparison with other studies or proper citation of references in the text.

